- AI Platform
- Data Engineering
- Industrial AI
- AI Platform
- AI Technology
- Advanced AI Learning
- AI Publication
- AI Applied in Finance
- Master AI
- AI Development Infrastructure Setup Guide
- Supervised Machine Learning Implementation Guide
- Unsupervised Machine Learning Implementation Guide
- Reinforcement Machine Learning Implementation Guide
- Deep Learning Implementation Guide
- Advanced Reinforcement Learning Implementation Guide
- Clients
- company
- Get Started
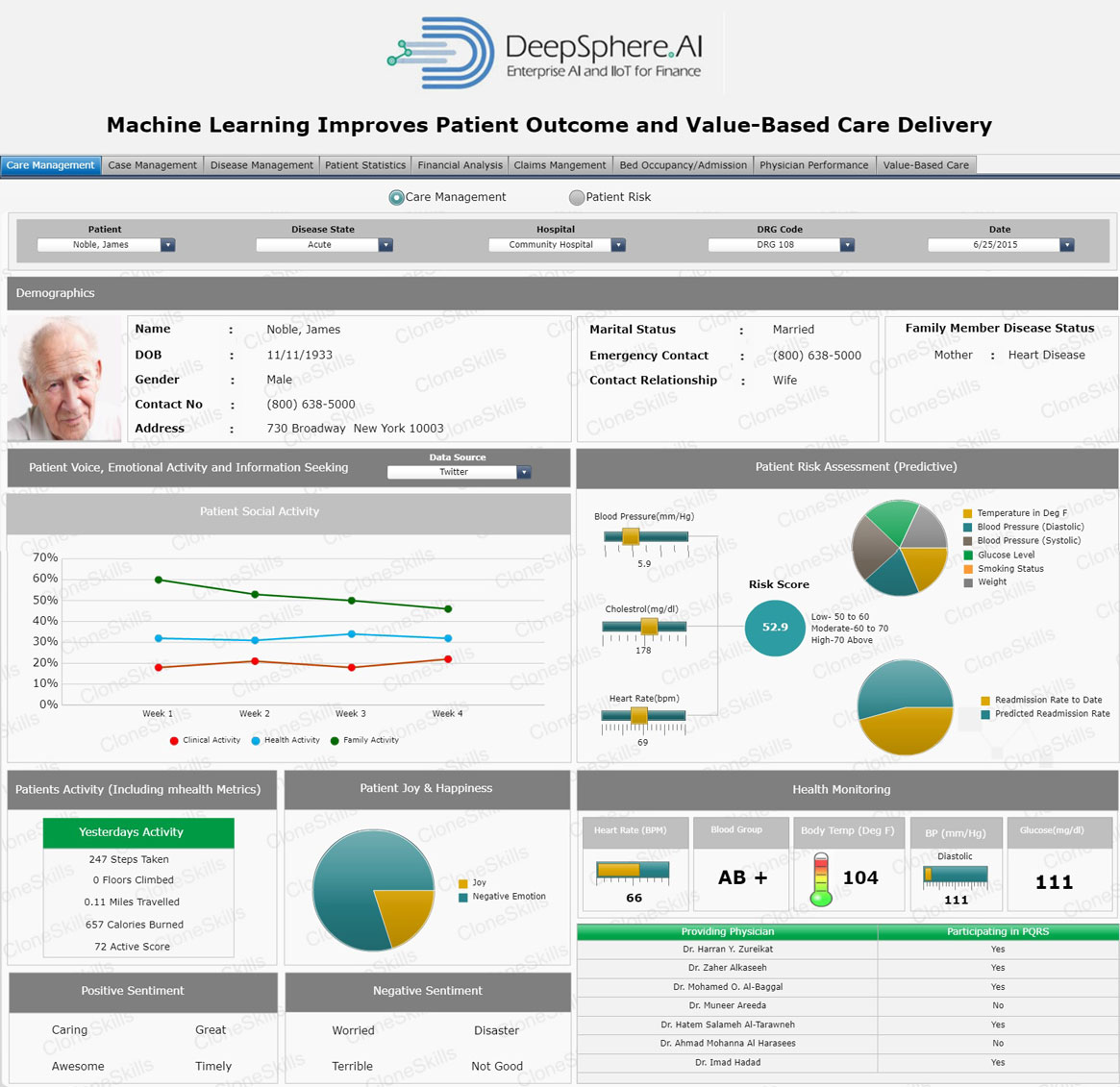
Patient Risk Score
Business Context
At its fundamental level “Patient Risk score” is a standardized metric for the likelihood that an individual will experience a particular health outcome. Risk score is a foundational technique for any successful population health management program. In healthcare, these outcomes can include service utilization events, such as hospital admissions, emergency department visits; or it could be the development of a certain clinical state, such as heart disease, diabetes, cancer, or sepsis.
Organizations develop risk scores by examining large cohorts of patients with similar characteristics, extracting key clinical and lifestyle indicators from them, and using algorithms to chart how those factors influence ultimate outcomes. They then compare other patients exhibiting similar clinical patterns to the validated historical data, which may help predict what will happen in the future.
Risk Score indicates the likelihood of a single event, such as a hospital readmission within the next six months. Healthcare payers and providers both use risk scores to estimate costs, target interventions, gauge a patient’s health literacy and lifestyle choices with the objective to prevent patients from developing more serious conditions that could result in higher spending and worse outcomes.
AI Model Details
- Linear Regression
- Polynomial Regression
- Decision Tree Regression
- Artificial Neural Networks
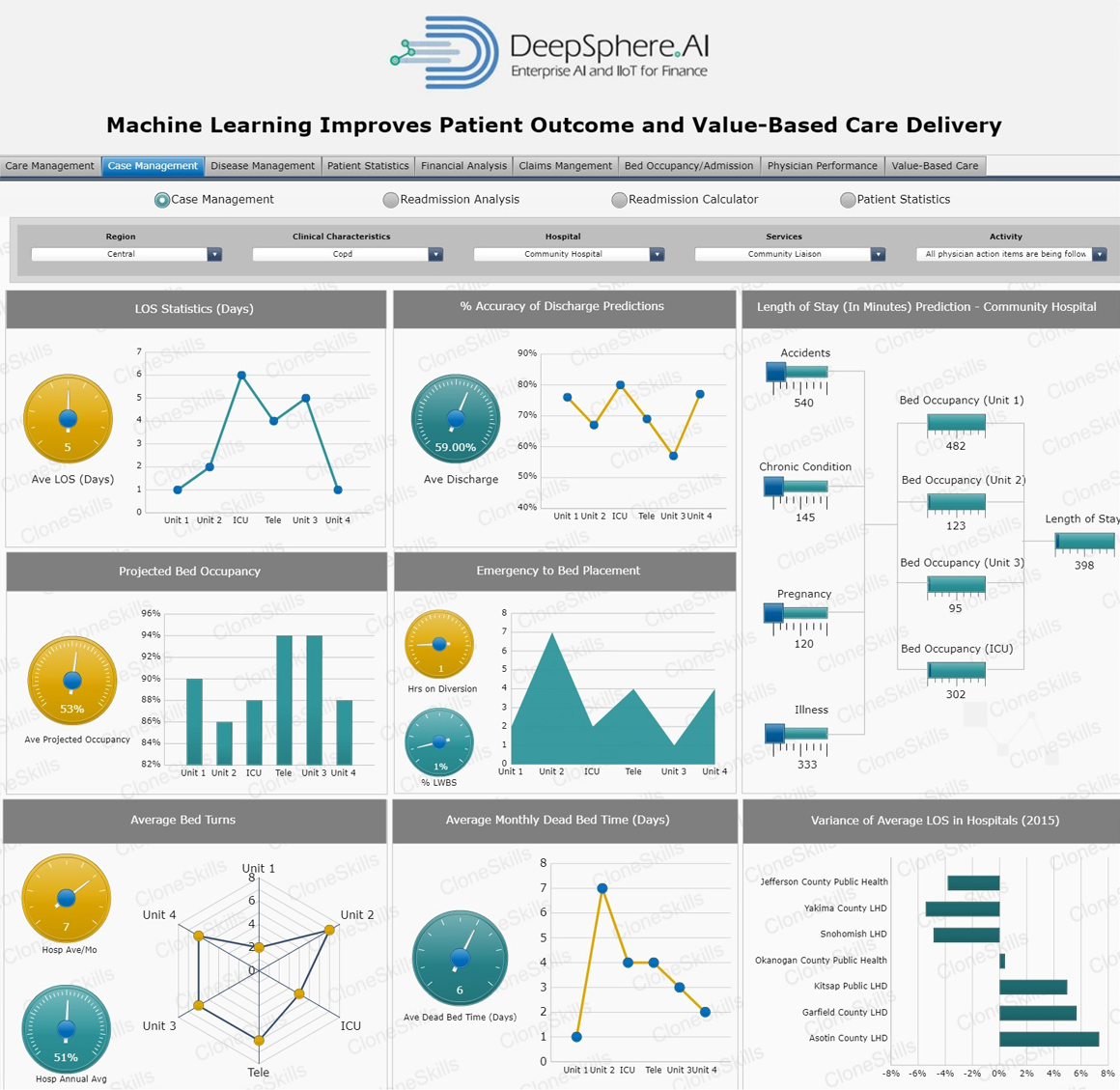
Length of Stay (LOS)
Business Context
“Length of Stay” (LOS) is a term coined as length of an inpatient episode of care, calculated from the day of admission to the day of discharge, based on the number of nights spent in the hospital. Patients admitted for one day are discharged on that same day.
Length of Stay (LOS) is calculated for new admissions to a nursing center from a hospital. New admissions are defined as any admission from a hospital with no assessments within the 100 days prior to the admission assessment. Each person’s LOS is calculated based on the number of days between their admission and discharge from the Center. If they are not discharged from the center within 120 days from admission they are assigned, a LOS of 120 days is designated, even if they stay past 120 days. The time frame is measured within 12 months rolling and updated quarterly.
Example: When an individual has an interruption in service that is 10 days or less, their LOS from their subsequent readmission to the Skilled Nursing Facility will be added to their prior admission’s LOS. For example, a person is admitted to a skilled nurrsing Facility on March 1st from a hospital and is sent back to the hospital on March 20th. Sheremains in the hospital for 6 days and is readmitted back to the skilled nursing facility on March 16th and remains in the skilled nursing facility for another 92 days. Her LOS would count as 114 days (10 days + 94 days).
AI Model Details
- Polynomial Regression
- Lasso Regression
- Ridge Regression
- Gradient Boosted Regression
Discharge Rate
Business Context
“Hospital Discharge Rate” is defined as the measure of number of patients who leave a hospital after receiving care. Hospital discharge is also defined as the release of a patient who has stayed at least one night in hospital. It includes deaths in hospital following inpatient care. Same-day discharges are usually excluded. This indicator is measured per 100 000 inhabitants.
A hospital discharge occurs when a hospital patient is formally released after an episode of care. The reasons for discharge include finalization of treatment, signing out against medical advice, transfer to another healthcare institution, or because of death.
Hospital care is for people who need a high level of medical attention. It is also expensive, and often uncomfortable. Being in the hospital also exposes one to the possibility of infection, particularly those with a weak immune system. Once a person is getting better and does not need a high level of care, a hospital stay is not needed. When the person is discharged, her bed becomes available to another person who needs a high level of care.
AI Model Details
- Lasso Regression
- ElasticNet Regression
- Ridge Regression
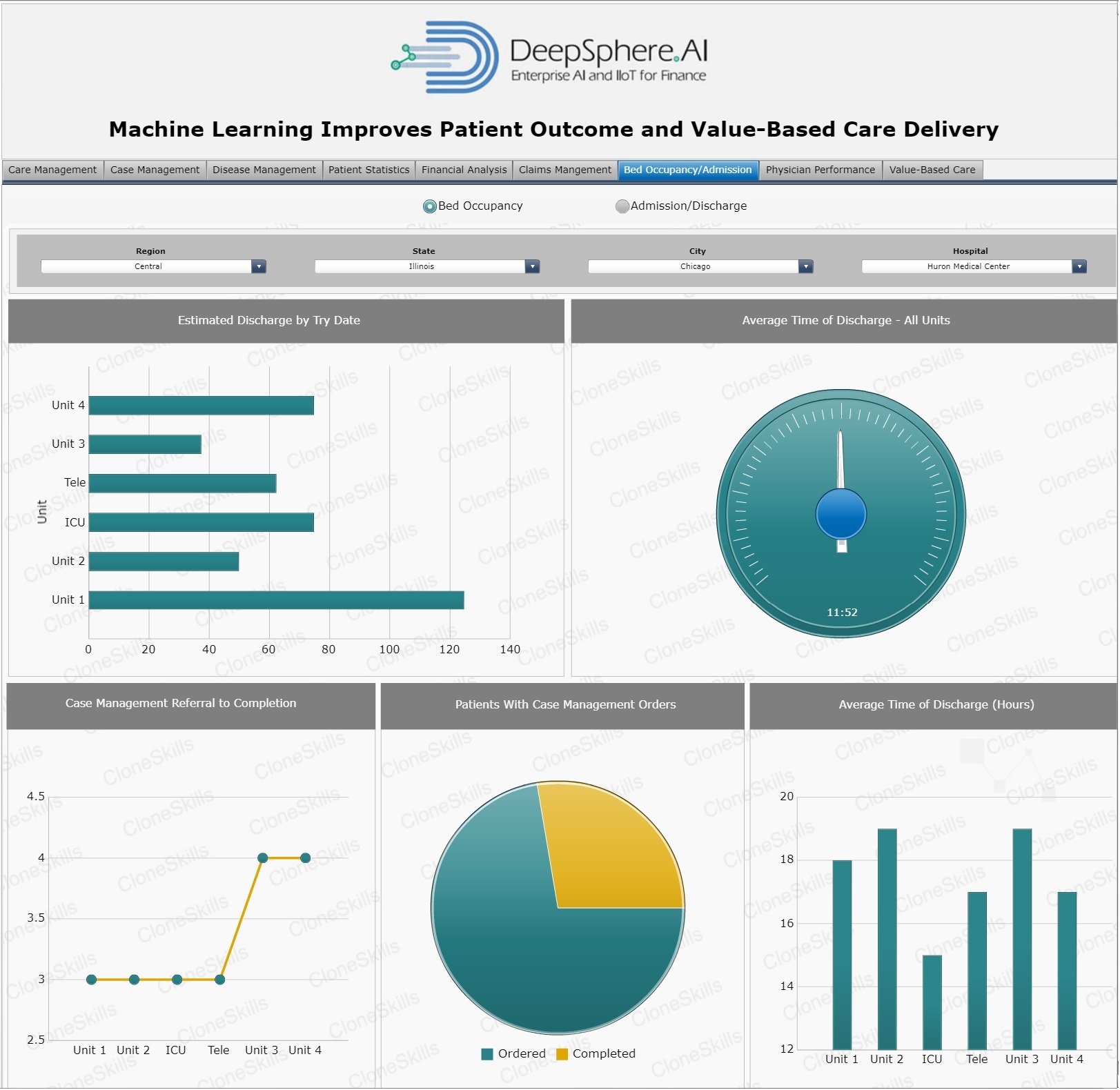
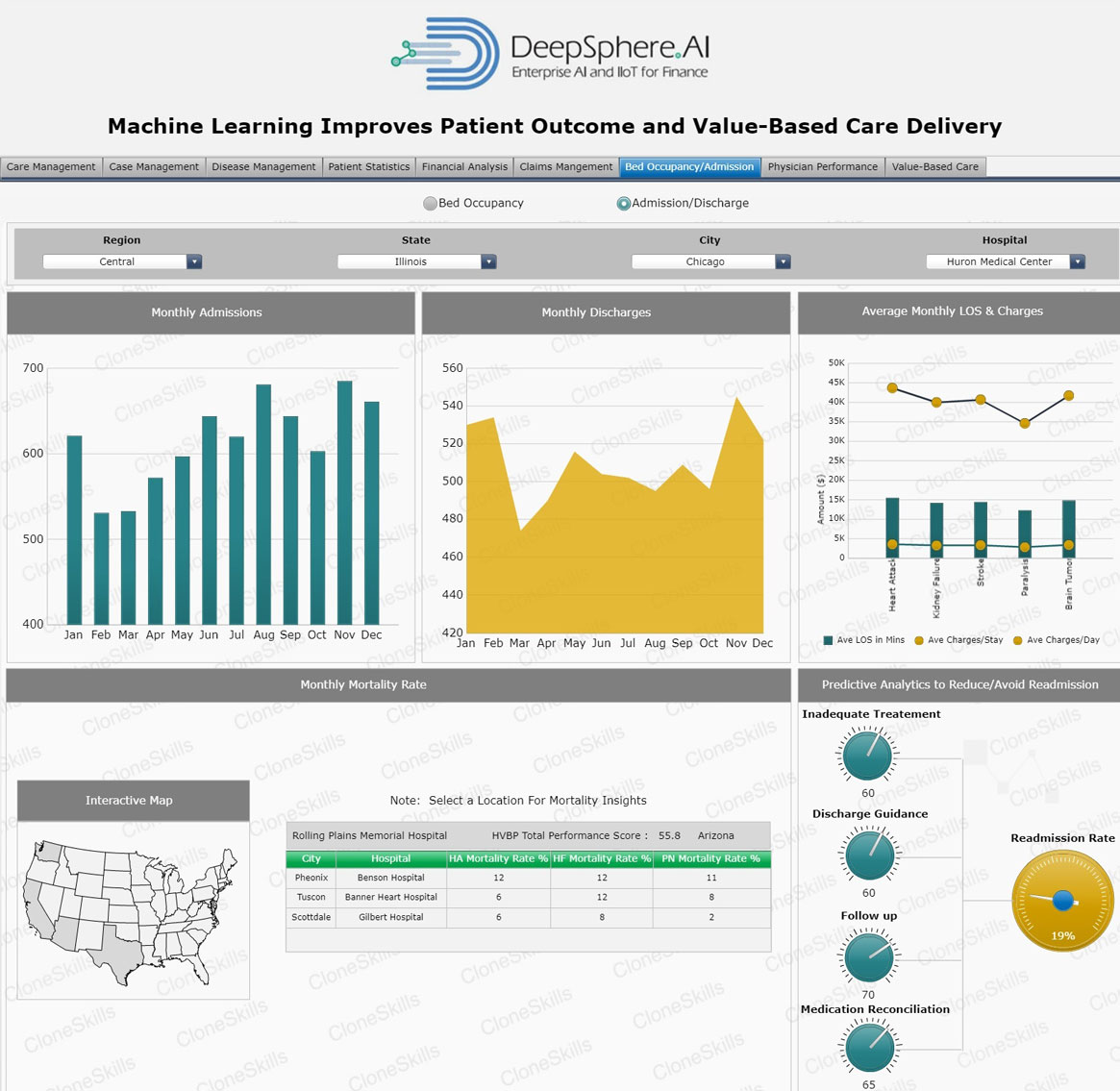
Bed Occupancy Rate
Business Context
“Bed Occupancy Rate” is a calculation used to show the actual utilization of an inpatient health facility for a given time period. It is expressed as a percent. Other terms often used synonymously include, “percent occupancy,” “percentage of occupancy,” or “occupancy ratio.” The occupancy rates are routinely calculated for hospitals and nursing homes and aggregated at the facility, county and state level. This information is very useful for health planning purposes and is requested from the Bureau frequently.
Bed occupancy rate reflects the popularity of the hospitals in terms of inpatients. The level of occupancy also varies with the type of facilities available in the hospital. Usually the number available of beds is in direct proportion to the number of doctors. As a result, more facilities are needed and the level of medical care tends to be of a higher magnitude. Therefore, it the bed occupancy ratio in district hospitals is typically higher than the bed occupancy ratio in the area and community health centers.
The bed occupancy rate, and in general, the utilization of hospitals is also set to vary with the medical facilities available in the private sector.
AI Model Details
- Stepwise Regression
- Gradient Boosted Regression
- Decision Tree Regression
- Artificial Neural Networks
Bed Turnover Rate
Business Context
“Hospital Bed Turnover Rate” denotes the number of times each hospital bed changed occupants make use of available hospital beds and has been defined as a measure of productivity. A lower rate may be due to high average length of stay; however, when both are very low, it might imply either underutilization or overcapacity. Bed Turnover Rate is measured by dividing the total discharges (including deaths) by the total number beds. Because it seems to be of less effect on the dependent variable, its coefficient is expected to be negative. A good hospital management includes an effective allocative planning for beds in a hospital. Bed occupancy rates and length of stay are the measures that reflect the functional ability of a hospital.
Hospital Bed Turnover Rate Indicates:
- An Important measure of Hospital Utilization Indices.
- Gives the net effect of changes in Occupancy Rate & Average Length of Stay at the hospital.
AI Model Details
- Ridge Regression
- Polynomial Regression
- Stepwise Regression
- ElasticNet Regression
Dead Bed Time
Business Context
The term “Hospital Dead Bed Time” is defined as the time which a bed remains unoccupied/vacant after previous Inpatient Discharge. Ideally, the movement of patients from admission through treatment and on to discharge should occur without significant delays. However, a department-centric or provider-centric environment focuses on the needs of individual areas, and one area’s needs are not necessarily compatible with another area’s priorities. For instance, nurses on a medical/surgical unit may not notify bed management that a bed has been vacated or may do so only after a substantial delay because such notifications are not a high priority for the medical/surgery unit. This can lead to a situation in which there are vacant beds that could be occupied by patients who may be kept waiting somewhere else, including hallways or the emergency department.
AI Model Details
- Linear Regression
- Ridge Regression
- Lasso Regression
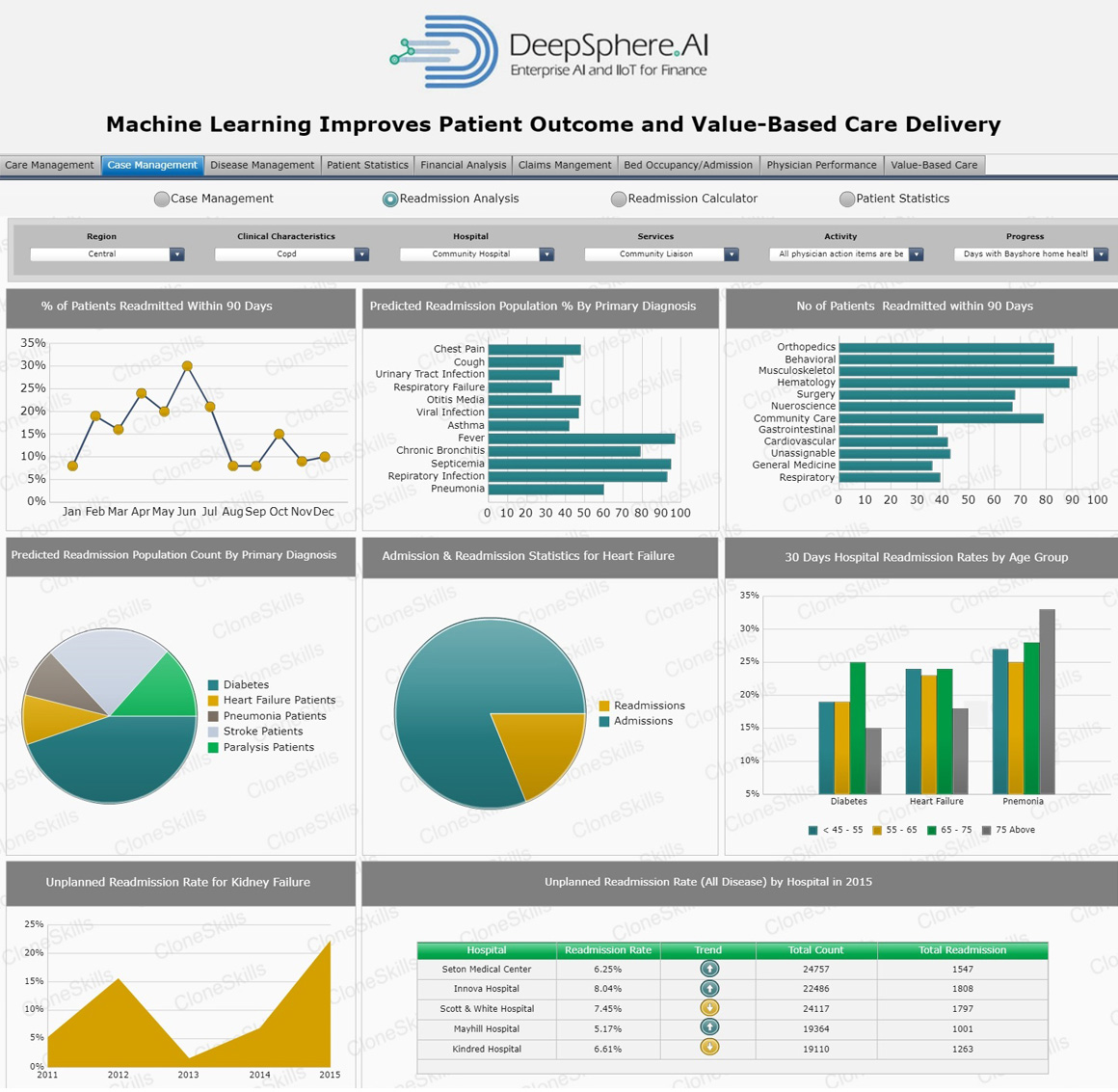
Readmission Rate
Business Context
“Patient Readmission Rate” is defined as percentage of patient admission to a hospital within 30 days after being discharged from an earlier hospital stay. Patients transferred to another hospital for longer term care will not count as a readmission. The percentage of admitted patients who return to the hospital within seven days of discharge will stay the same or decrease as changes are made to improve patient flow through the system.
Percentage of readmitted patients is an important balancing measure to indicate if changes to patient flow through the system are negatively affecting care. While some readmissions are part of the planned care and are desirable, others may be indications of a quality issue related to shortened length of stay and premature discharge.
Tracking the number of patients who experience unplanned readmissions to a hospital after a previous hospital stay is one category of data used to evaluate the quality of hospital care. It’s important to note that unplanned hospital readmissions may or may not be related to the previous visit, and some unplanned readmissions aren’t preventable. Whatever the reason, insurance companies and other payers sometimes view unplanned hospital readmissions as wasteful spending.
AI Model Details
- ElasticNet Regression
- Decision Tree Regression
- Artificial Neural Networks
- Recurrent Neural Networks
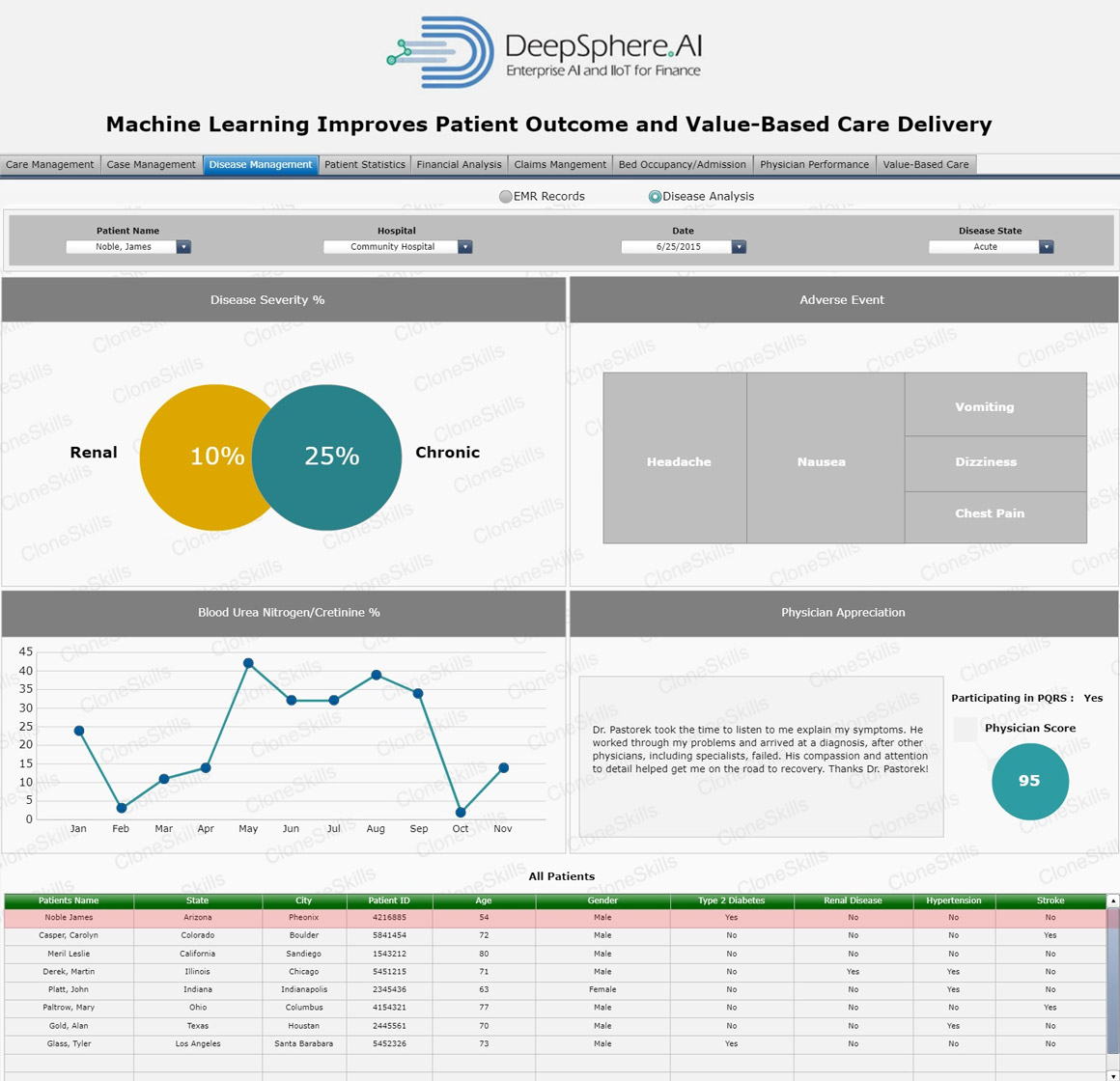
Patient Disease Condition
Business Context
A ”Disease” is a particular abnormal condition that negatively affects the structure or function of part or all of an organism, and that is not due to any external injury. Diseases are often construed as medical conditions that are associated with specific symptoms and signs. A disease may be caused by external factors such as pathogens or by internal dysfunctions. For example, internal dysfunctions of the immune system can produce a variety of different diseases, including various forms of immunodeficiency, hypersensitivity, allergies and autoimmune disorders.
Disease Conditions are of the following types:
- Acute: An acute disease is one of a short-term nature (acute); the term sometimes also connotes a fulminant nature.
- Chronic: A chronic disease is one that persists over time, often characterized six months or more.
AI Model Details
- Naïve Bayes
- K-Nearest Neighbors
- Random Forest
- Decision Tree
Patient PQRS Participation
Business Context
“Physician Quality Reporting System” (PQRS) is the largest quality-reporting system in the U.S. health care system and a basis for the new value-based modifier system for physician payment. The PQRS allows health care providers to report measures of quality of care that include both the process of care and physiological outcomes.
The PQRS is one of several long-term quality initiatives developed by the Centers for Medicare and Medicaid Services (CMS). It is intended to, among other things; obtain information on the quality of care across the healthcare system. Specifically, the program collects data submitted by Eligible Professionals (EP), on quality measures for covered services provided to Medicare part B fee for service (FFS) beneficiaries.
Participating in the PQRS is not mandatory, it is voluntary. However, the program uses a combination of incentive payments and payment adjustments to promote reporting of quality information by EPs. Those who participated and successfully met the measure reporting criteria of the program receive incentive payments (bonus). EPs that decided not to report measures, or did not meet the programs’ reporting criteria, were subject to payment adjustments (penalty). The table below describes the incentive/adjustment payment schedule.
AI Model Details
- Naïve Bayes
- Logistic Regression
- Random Forest
- Decision Tree
Physician Appreciation Score
Business Context
A “Physician Appreciation Score” is defined as Appreciation Score given to a physician based on the level of interaction with the patient. Physician quality measures can be used to evaluate the performance of an individual physician or groups of physicians that practice together (such as a pediatric group practice). However, while patients have indicated a preference for quality information at the level of individual physicians, most current information is at the level of medical groups.
The advantage of constructing appreciation scores at the group level is the availability of a larger patient population. When measuring quality at the medical group level, one can create a sample by combining patient data from each physician in the group. It is more difficult to produce adequate sample sizes for individual physicians without a sufficient number of patients with the disease or condition addressed by the measure. The minimum number of required observations needed to calculate a score for an individual performance measure varies. Recommendations range from 30 to 50 patients per physician. However, a larger sample is often necessary depending on the characteristics of the measure or data source.
AI Model Details
- Ridge Regression
- Decision Tree Regression
- Lasso Regression
- Stepwise Regression
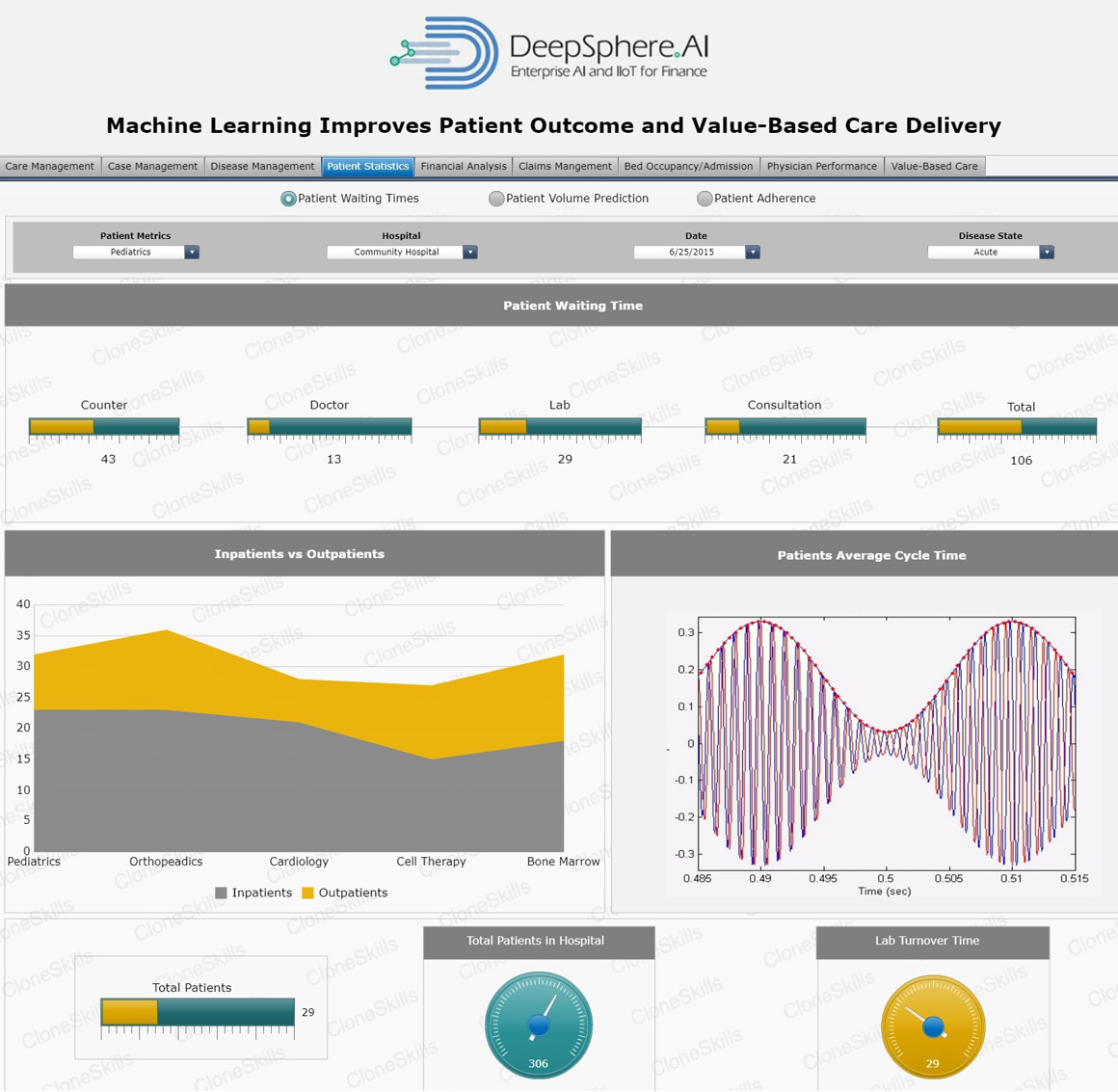
Patient Waiting Time
Business Context
“Patient Waiting Time” refers to the time a patient waits in the clinic before being seen by one of the clinic medical staff. Patient clinic waiting time is an important indicator of quality of services offered by hospitals. The amount of time a patient waits to be seen is one factor which affects utilization of healthcare services. Patients perceive long waiting times as a barrier to actually obtaining services. Keeping patients waiting unnecessarily can be a cause of stress for both patient and doctor. Waiting time is a tangible aspect of practice that patients will use to judge health personnel, even more than their knowledge and skill.
Time spent waiting is a resource investment by the patient for the desired goal of being seen by the physician and therefore may be moderated by the outcome. Various factors contributing long waiting time are registration clerk not attending duty on time, taking more time to register the patient, difficulties in locating rooms, rush, doctors coming late on duty, doctors, pharmacists talking on mobiles, VIP patients jumping queue etc. Association is observed between waiting time and total satisfaction and between times spent with doctor and total satisfaction.
Improving patient’s satisfaction towards health care services can be accomplished by reducing their waiting time, attending the patient in a timely and empathetic manner will result in patient satisfaction and credibility for the hospital within a community.
AI Model Details
- Polynomial Regression
- Lasso Regression
- ElasticNet Regression
Inpatient & Outpatient
Business Context
An “Inpatient” is someone who’s been admitted to hospital for medical treatment. The main two ways that one can become an inpatient is through a hospital’s ER (emergency room), or through a pre-booked surgery or treatment. One does not have to stay overnight in a hospital to be classified as an inpatient, so as long as one has been admitted by a doctor and received treatment, such as surgery or an endoscopy, even if one stays in for the day. That person will still be classified as an inpatient. It is important to remember that even while visiting with your doctor or specialist at a hospital, you are not automatically classified as an inpatient. Some medical professionals may have a room they work from within a hospital.
One may be classified as an “Outpatient” for any sort of medical treatment in a doctor’s surgery, specialist’s clinic or even in a hospital’s emergency room where one has not been admitted to hospital. So, even if a patient has been previously admitted to the hospital as an inpatient. One is automatically classified as anoutpatient, once discharged.
AI Model Details
- Lasso Regression
- Polynomial Regression
- Gradient Boosted Regression
- Decision Tree Regression
Laboratory Turnaround Time
Business Context
The “Laboratory Turnaround Time” is defined as the time from when a test is ordered until the result is reported. Laboratory Turnaround time is one of the most noticeable signs of laboratory service and is often used as a key performance indicator of laboratory performance.
Rapid laboratory turnaround is important from a cultural, medical, logistical, and commercial perspective. When turnaround time does not meet customers’ expectations, they frequently let laboratory management know about their problem. More than four fifths of hospital-based laboratories receive complaints about test turnaround time.8 Pressure to discharge inpatients as quickly as possible, and intense competition in the outpatient testing marketplace, are likely to heighten clinicians’ demands for more rapid laboratory turnaround time in the future.
AI Model Details
- Stepwise Regression
- Decision Tree Regression
- Lasso Regression
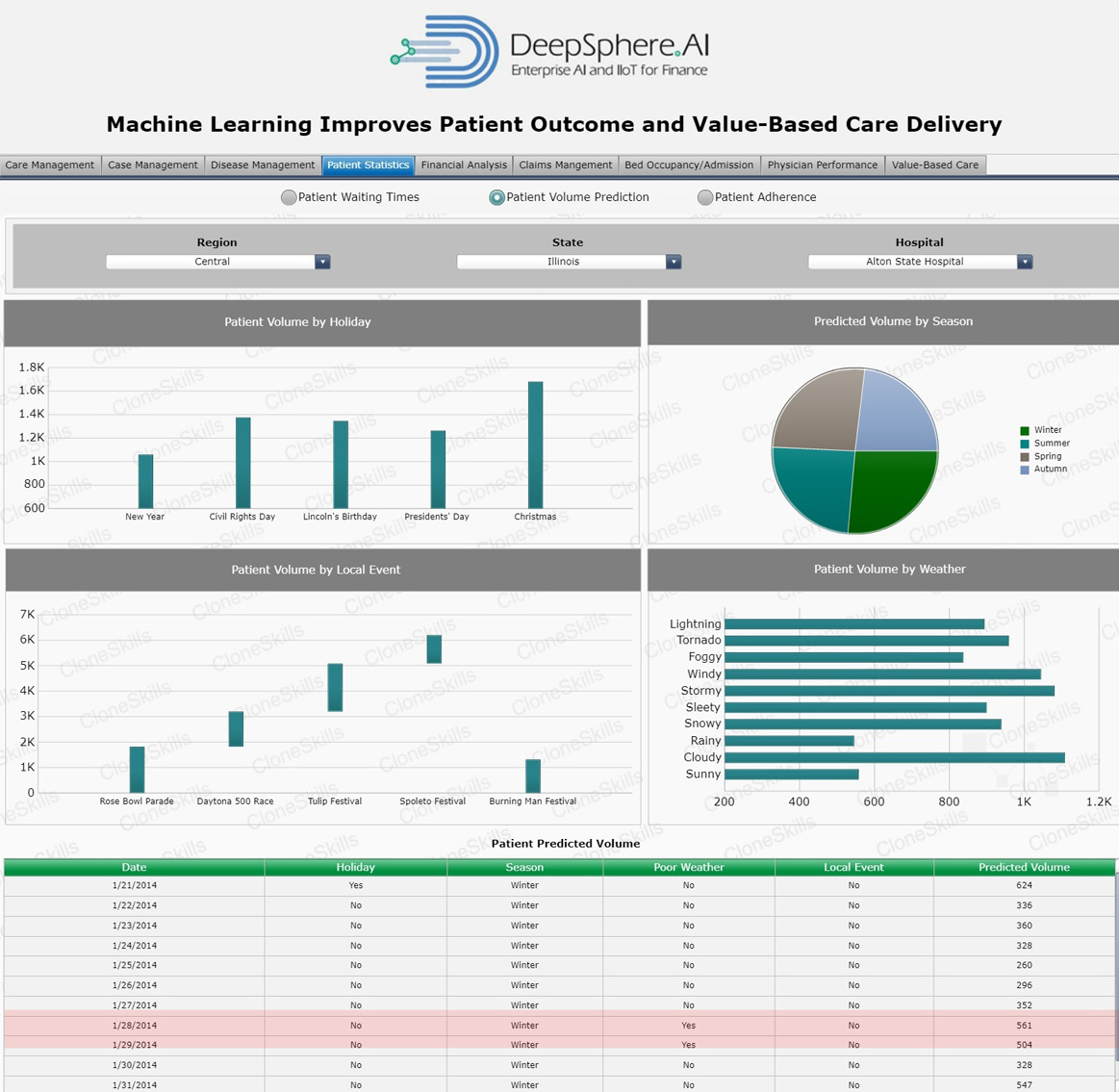
Patient Volume
Business Context
The term “Patient Volume” is defined as the number of cases of specific conditions (such as stroke, acute myocardial infarction, or organ transplantation) treated at an inpatient facility. Morbidity and mortality are typically lowest in treatment centers where professional staff has the greatest clinical experience.
The performance of a hospital is linked to the patient volume of various surgical procedures and medical conditions. Generally, high-volume hospitals have shown to be more efficient and have better outcomes than low-volume hospitals. Documentation of the volume-outcome relationship is important because patient outcomes may be improved through volume-based selective referral.
AI Model Details
- Ridge Regression
- Linear Regression
- Polynomial Regression
- Artificial Neural Networks
Medication Adherence Rate
Business Context
The term “Medication Adherence Rate” is typically defined as the percentage of patients taking medications correctly and as prescribed. This includes taking the correct dosage at the right time(s) each day and getting prescriptions refilled in a timely fashion.
Cost and poor understanding of the directions for the treatment, referred to as ‘health literacy’ have been known to be major barriers to Medication Adherence. There is robust evidence that education and physical health are correlated. Poor educational attainment is a key factor in the cycle of health inequalities. Poor Medication Adherence can adversely affect the trajectory of a disease, and the increase in medical services necessary to ameliorate those effects can be costly. This is problematic, as poor adherence leads to both sub-optimal clinical benefits for patients as well as an inefficient use of health care resources. Due to many factors and complexities underlying poor drug adherence, interventions to increase patient drug adherence have proven a challenge.
AI Model Details
- Decision Tree Regression
- Linear Regression
- Polynomial Regression
- Artificial Neural Networks
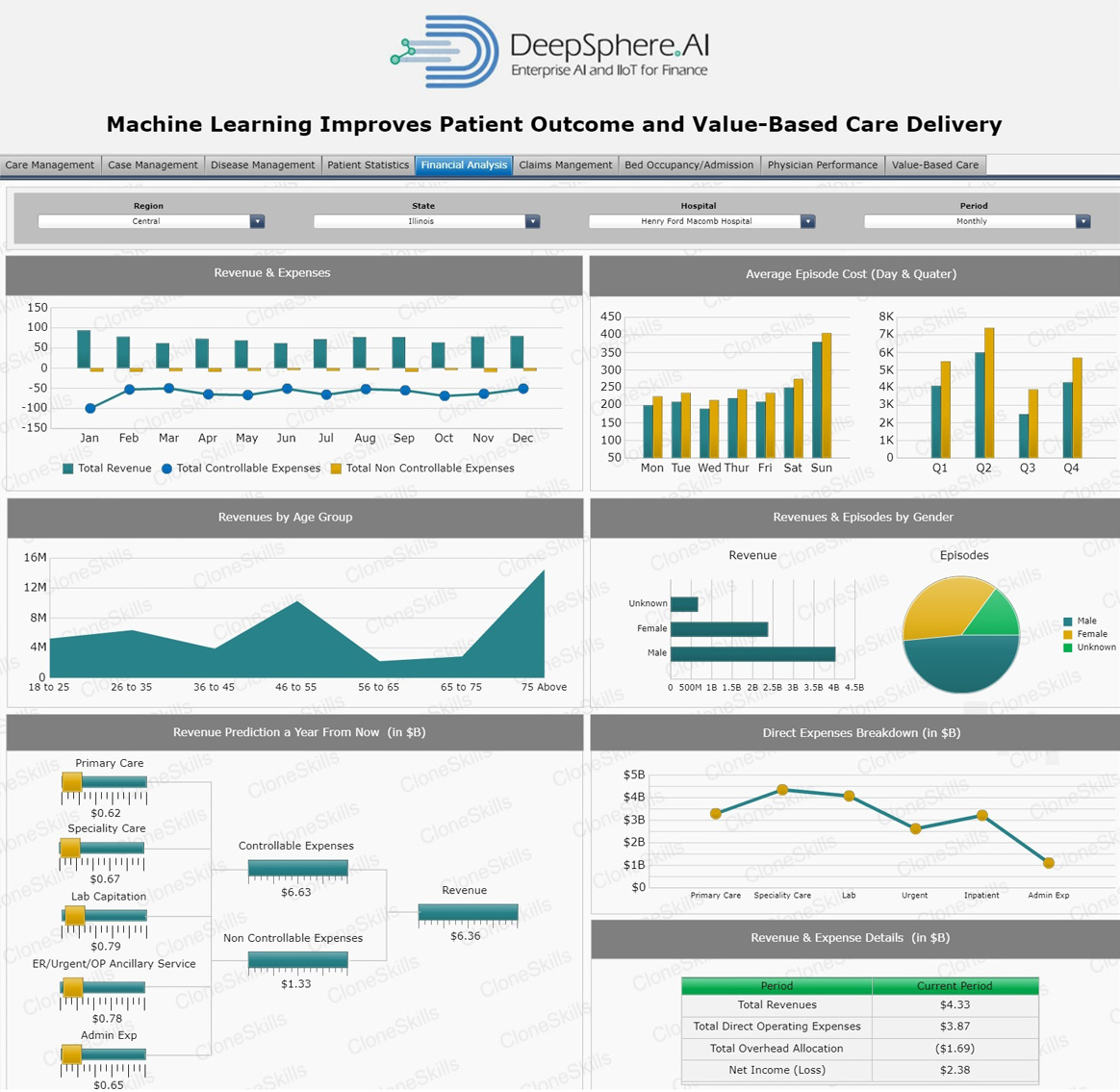
Revenue & Expenses
Business Context
“Hospital Revenue” is a term that includes the entire life of a patient account from creation to payment. A Hospital Revenue cycle processes flow into and affect one another. When processes are executed correctly, the cycle performs predictably. However, problems early in the cycle can have significant ripple effects. The further an error travels through the revenue cycle, the more costly revenue recovery becomes.
“Hospital Expenses” are any costs incurred in the prevention or treatment of injury or disease. Hospital expenses include health and dental insurance premiums, doctor and hospital visits, co-pays, prescription and over-the-counter drugs, glasses and contacts, crutches and wheelchairs, to name a few. Hospital expenses that are not reimbursed are deductible within certain limits.
Supplies make up about 15 percent of the average hospital’s expenses. Of course, these costs are offset through billing to patients for supplies used in the course of their treatment. Capital expenditures can be a huge part of a hospital’s outlays. However, the amount and percentage of the budget can vary dramatically by hospital. A hospital undergoing a major expansion or construction project may have very large capital expenditures, while other hospitals may buy just a few new pieces of equipment, making their annual capital expenses fairly low. Nonprofit hospitals often fund capital-expense budgets for expansions and facility renovations through donations, and therefore the expenses do not come from their general operating budgets.
AI Model Details
- ElasticNet Regression
- Ridge Regression
- Polynomial Regression
- Linear Regression
Revenue & Expenses
Business Context
“Hospital Revenue” is a term that includes the entire life of a patient account from creation to payment. A Hospital Revenue cycle processes flow into and affect one another. When processes are executed correctly, the cycle performs predictably. However, problems early in the cycle can have significant ripple effects. The further an error travels through the revenue cycle, the more costly revenue recovery becomes.
“Hospital Expenses” are any costs incurred in the prevention or treatment of injury or disease. Hospital expenses include health and dental insurance premiums, doctor and hospital visits, co-pays, prescription and over-the-counter drugs, glasses and contacts, crutches and wheelchairs, to name a few. Hospital expenses that are not reimbursed are deductible within certain limits.
Supplies make up about 15 percent of the average hospital’s expenses. Of course, these costs are offset through billing to patients for supplies used in the course of their treatment. Capital expenditures can be a huge part of a hospital’s outlays. However, the amount and percentage of the budget can vary dramatically by hospital. A hospital undergoing a major expansion or construction project may have very large capital expenditures, while other hospitals may buy just a few new pieces of equipment, making their annual capital expenses fairly low. Nonprofit hospitals often fund capital-expense budgets for expansions and facility renovations through donations, and therefore the expenses do not come from their general operating budgets.
AI Model Details
- ElasticNet Regression
- Ridge Regression
- Polynomial Regression
- Linear Regression
Direct Expenses
Business Context
In Health Economics term “Direct Expenses” refers to all expenses due to resource use that are completely attributable to the use of a health care intervention or illness. Direct Expenses can be split into direct medical expenses and direct non-medical expenses. Direct medical expenses include the expense of a defined intervention and all follow-up Expense for other medication and health care interventions in ambulatory, inpatient, and nursing care. All specialist and GP care, including emergency care, as well as rehabilitation and physiotherapy, is considered. Direct non-medical expenses include transportation costs and additional paid caregiver time.
Direct Expenses involve a transaction for medical services, including things such as physician services, diagnostic tests, and hospitalization expenses. When analyzing expenses from a payer perspective (e.g., insurance company), these expenses are most important.
However, from a patient’s perspective, it is the actual out‐of‐pocket expenses that are meaningful (i.e., expenses not covered by insurance). The patient is the individual who “receives” the medical goods. These expenses may be direct out‐of‐pocket expenses (direct nonmedical expense) or expenses from indirect consequences of an illness (indirect expense). Indirect Expenses are the lost earnings and productivity by the patient or caregivers related to the morbidity and mortality of illness.
AI Model Details
- Gradient Boosted Regression
- Polynomial Regression
- Decision Tree Regression
Episode of Care Costs
Business Context
In Health Economics term an “Episode of Care Costs” are the costs that covers all the care a patient receives in the course of treatment for a specific illness, condition or medical event. Examples of episodes of care for which a single, bundled payment can be made include all physician, inpatient and outpatient care for a knee or hip replacement, pregnancy and delivery, or heart attack.
Episode of care savings can be realized in three ways: 1) Negotiating a payment so the total cost will be less than fee-for-service; 2) Agreeing with providers that any savings that arise because total expenditures under episode-of-care payment are less than they would have been under fee-for-service will be shared between the payer and providers; and/or 3) Savings that arise because no additional payments will be made for the cost of treating complications of care, as would normally be the case under fee-for-service.
Episode of care costs also are known as case rates, evidence-based case rates, condition-specific capitation and episode-based bundled payments. Some episodes of care represent a higher risk than others. Additionally, patients also represent different levels of risk based on age, behavioral factors, and comorbidities. For these reasons, bundles can be adjusted to reward providers who assume more risk.
AI Model Details
- Linear Regression
- Polynomial Regression
- Artificial Neural Networks
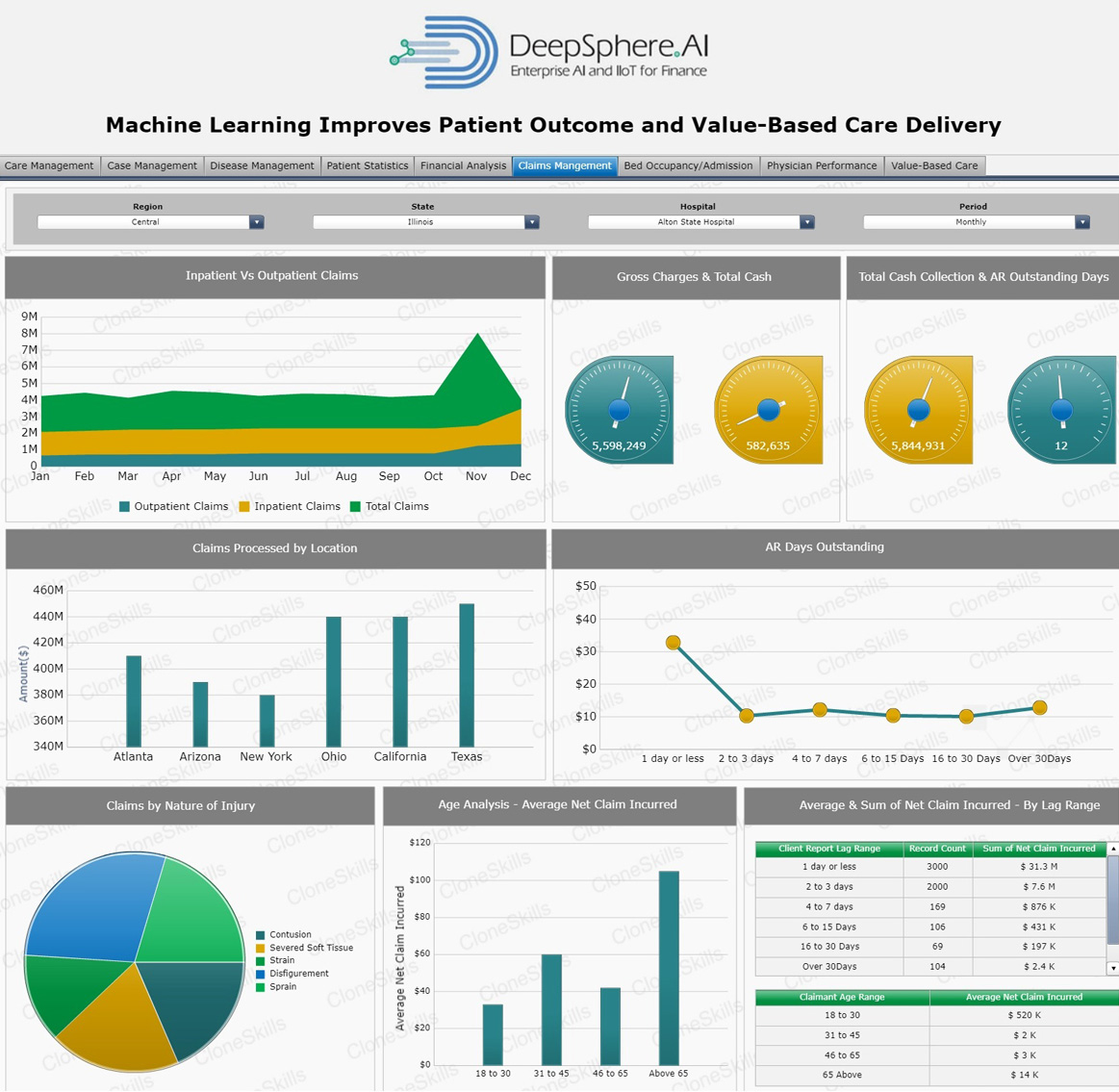
Inpatient Claims
Business Context
Inpatient refers to a person who has been admitted to an approved hospital or day surgery facility and discharged following treatment. If you have been admitted as a private inpatient you will be able to claim benefits for the services listed in your chosen level of hospital cover. This is Procedure is termed “Inpatient Claims”.
AI Model Details
- Stepwise Regression
- Linear Regression
- Polynomial Regression
- ElasticNet Regression
Outpatient Claims
Business Context
Outpatient refers to a patient who has received medical treatment in a doctor’s surgery or emergency department and has not been admitted into hospital. In this instance you would not be covered by private health insurance. These services may be eligible for claims through Medicare. Services include X-rays, blood tests and MRI’s. This procedure is termed “Outpatient Claims.”
AI Model Details
- Lasso Regression
- ElasticNet Regression
- Decision Tree Regression
- Gradient Boosted Regression
Accounts Receivables (AR) Days
Business Context
In health economics, “Outstanding Accounts Receivables (AR) Days” is defined as the average number of days it takes to collect the payments due to the practice.
For example, if a patient is charged $280,000 within the past six months, and if there were 182 days in those months, the average daily revenue is $1,538. Then, the total accounts receivable is $70,000. The days in Accounts Receivable is 45.5 because it takes an average of 45.5 days to collect patients’ payments.
Days in accounts receivable measure the amount of time between patient discharge and when payment is made. This directly impacts cash flows for the facility. The quicker the turnover in accounts receivable, the less cash is available somewhere else. The ultimate aim is minimizing the lag between claim submission and when the payment for those services is received. A/R days measure how well you are completing that objective.
AI Model Details
- Linear Regression
- Polynomial Regression
- Lasso Regression
- Artificial Neural Networks
Estimated Dicharges
Business Context
“Discharge” from the hospital is the point at which the patient leaves the hospital and either returns home or is transferred to another facility, such as rehabilitation or to a nursing home. Discharge involves the medical instructions that the patient will need to fully recover. Discharge planning is a service that considers the patient’s needs after the hospital stay and may involve several different services such as visiting nursing care, physical therapy, and home blood drawing.
Hospitalization is often a short-term event, so planning for discharge may begin shortly after admission. The physicians, nurses, and case managers involved in a patient’s care are part of an assessment team that keep in mind the patient’s pre-admission level of functioning and whether the patient will be able to return home following the current hospital admission. Information that could affect the discharge plan should be noted in the patient’s medical record so that it will be taken into account when discharge is being scheduled.
While a person is in the hospital, physicians other than those in primary care are in charge of the patient’s care. Good discharge planning involves clear communication between the hospital physician(s) and the primary care physician. This may be done by telephone and/or in writing.
AI Model Details
- Ridge Regression
- Stepwise Regression
- ElasticNet Regression
- Lasso Regression
Patient Mortality Rate
Business Context
“Patient Mortality Rate” or ”Patient Death Rate”, is a measure of the number of deaths (in general, or due to a specific cause) in a particular population, scaled to the size of that population, per unit of time. Mortality rate is typically expressed in units of deaths per 1,000 individuals per year. Thus, a mortality rate of 9.5 (out of 1,000) in a population of 1,000 would mean 9.5 deaths per year in that entire population, or 0.95% out of the total.
Mortality Rates are measured within 30 days, because deaths after a longer time period may have less to do with the care the hospital provided and more to do with other complicating illnesses, patients’ own behavior, or other care services patients received after they leave the hospital.
The Mortality rates include hospitalizations for Medicare beneficiaries 65 or older who were enrolled in Original Medicare for 12 months before their hospital admission. The death rates do not include patients who left the hospital against medical advice.
AI Model Details
- Linear Regression
- Stepwise Regression
- Gradient Boosted Regression
Physician Discharges & Collections
Business Context
“Physician Charges” are defined as the full, non-discounted fees charged for all services provided before any contractual, charitable, courtesy, bad debt, or other adjustments are applied. Because charges are unique to every practice or group, they are often thought to be meaningless in the context of revenue generation. While it is true that charges generally do not directly translate into revenue, it is rare that full charges are collected charges for physicians performing similar work on an even playing field.
“Physician Collections” is the actual cash received for services rendered. In many practices, cash received is recorded as the actual revenue so this method is directly tied to the bottom line. It is also relatively simple to capture this information by physician. However, this method may not accurately reflect the work performed.
AI Model Details
- Linear Regression
- Decision Tree Regression
- Gradient Boosted Regression
- Artificial Neural Networks
Patient Experience
Business Context
“Patient Experience” is defined as an individual’s experience of illness/injury and how healthcare treats them. Increasing focus on patient experience is part of a move towards patient-centered care. It is often operationalized through metrics, a trend related to consumerism and New Managerialism.
Patient experience has become a key quality outcome for healthcare. Measuring is a means of support improvement in healthcare quality, governance and public accountability. Patient experience encompasses the range of interactions that patients have with the health care system, including their care from health plans and from doctors, nurses, staff in hospitals, physician practices, and other health care facilities. As an integral component of health care quality, patient experience includes several aspects of health care delivery that patients highly value when they seek and receive care, such as getting timely appointments, easy access to information and good communication with health care providers.
Patient Experience is a key step in moving towards patient-centered care. By looking at various aspects of patient experience, one can assess the extent to which patients are receiving care that is respectful of and responsive to individual patient preferences, needs and values. Evaluating patient experience along with other components such as effectiveness and safety of care is essential to providing a complete picture of health care quality.
AI Model Details
- Linear Regression
- Lasso Regression
- Ridge Regression
Cost per Capita
Business Context
“Cost per Capita” is the sum of public and private health expenditures as a ratio of total population. It covers the provision of health services (preventive and curative), family planning activities, nutrition activities, and emergency aid designated for health but does not include provision of water and sanitation.
Cost per Capita measures the final consumption of health care goods and services (i.e. current health expenditure) including personal health care (curative care, rehabilitative care, long-term care, ancillary services and medical goods) and collective services (prevention and public health services as well as health administration), but excluding spending on investments. Health care is financed through a mix of financing arrangements including government spending and compulsory health insurance (“Government/compulsory”) as well as voluntary health insurance and private funds.
AI Model Details
- Polynomial Regression
- Linear Regression
- Stepwise Regression
- Ridge Regression
Quality of Care
Business Context
“Hospital Quality of Care” is defined as the extent to which health care services provided to individuals and patient populations improve desired health outcomes. In order to achieve this, health care must be safe, effective, timely, efficient, equitable and people-centered.
Health facilities often struggle to provide the rapid emergency care needed to manage maternal complications and care for small and sick newborns. Common causes include inadequate or unhygienic infrastructure; lack of competent, motivated staff; lack of availability or poor quality of medicines; poor compliance to evidence-based clinical interventions and practices; and poor documentation and use of information. Improving quality of care and patient safety are therefore critical if we want to accelerate reductions in maternal and newborn mortality.
Quality of care is also a key component of the right to health and the route to equity and dignity for women and children. In order to achieve universal health coverage, it is essential to deliver health services that meet quality criteria.
AI Model Details
- Linear Regression
- Polynomial Regression
- Ridge Regression
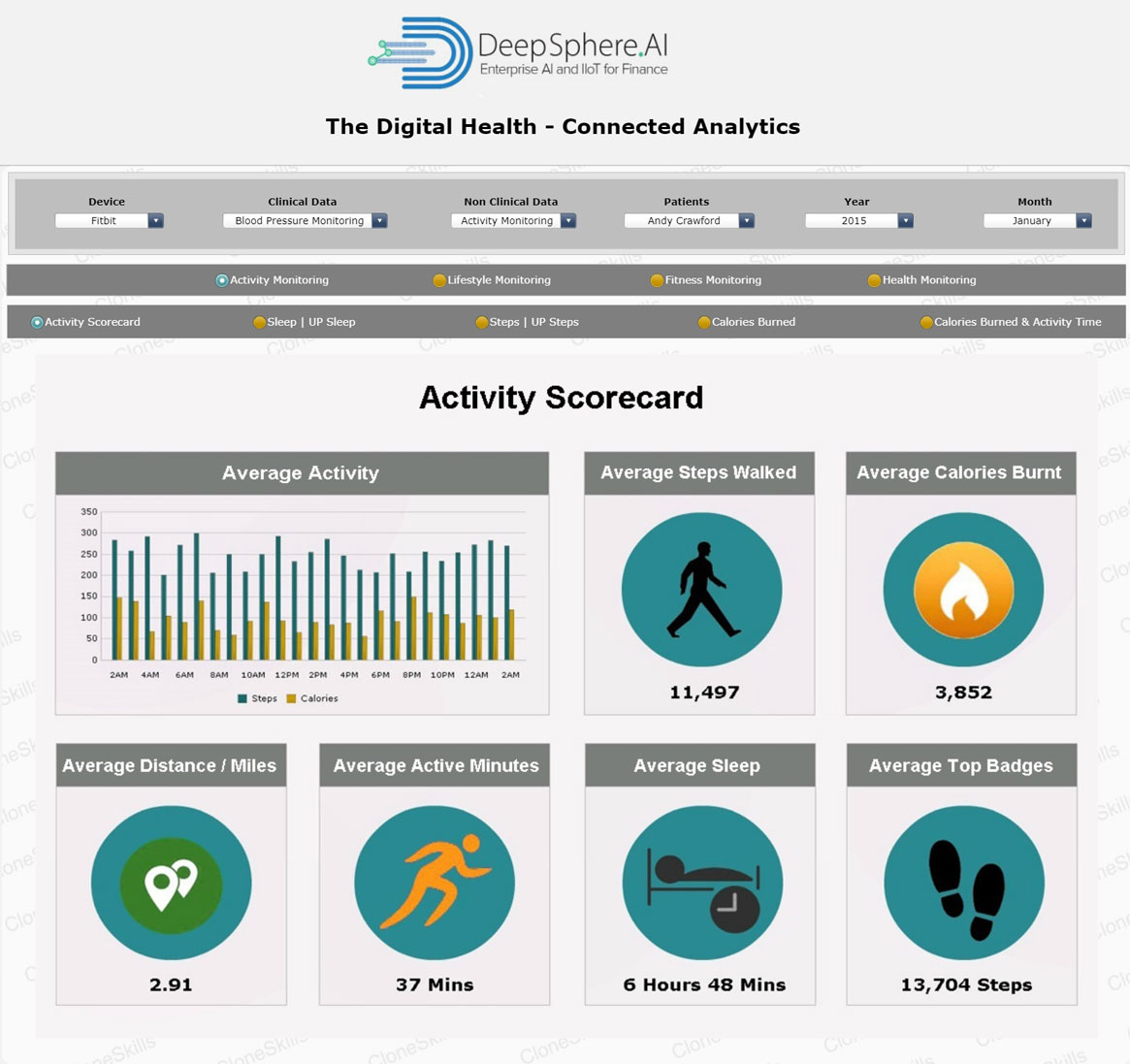
Steps Walked
Business Context
Walking is a great form of physical activity that is free, low-risk and easy to do. Specifically, it helps you lose weight and burn belly fat and calories. Burning calories can help you maintain or lose weight. Walking can offer numerous health benefits to people of all ages and fitness levels. It may also help prevent certain diseases and even prolong your life. “Steps Walked” can be defined as one’s goal to burn calories in a day.
Walking is the most popular physical activity among adults, and it is easy to see why. It requires no special clothes or equipment, and it is free. Regular walking can have many health benefits. It may lower your risk of high blood pressure, heart disease, and diabetes. It can strengthen your bones and muscles. It may help you maintain a healthy weight. It might also help lift your mood. One can make walking fun by going to places that bring joy, like a shopping center or a park. Bring along someone to chat with, or listen to some of your favorite music (but keep the volume low enough to hear the sounds around you).
If losing weight or preventing weight gain is your top concern, you may need even more moderate-intensive physical activity, such as walking 60 to 90 minutes of a few days during the week. Even a small increase in steps can make a difference in health for those who are normally sedentary. Walking as little as 6,000 steps per day correlate to a lower death rate in men. But 10,000 steps can be too challenging for people who are elderly, sedentary, or afflicted with chronic diseases.
AI Model Details
- Linear Regression
- Polynomial Regression
- Ridge Regression
- Lasso Regression
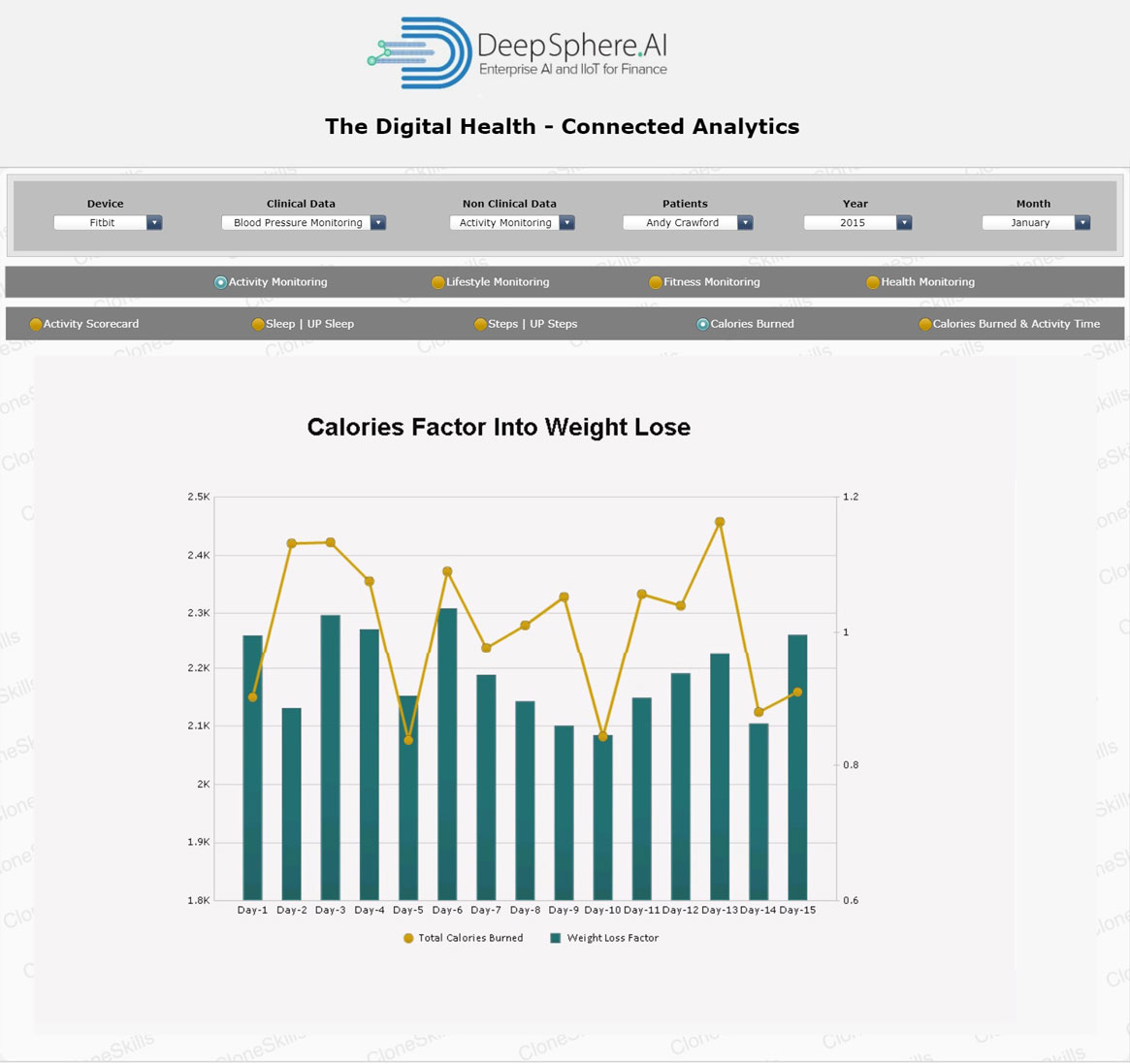
Calories Burnt
Business Context
Definition: Calorie is a measure of energy expenditure and stored energy. “Calories Burnt” can be seen as an act of weight loss. The number of calories that you burn in a day include basal metabolic rate which is calories burned just to keep the body functioning, plus additional calories burned in physical activity. Your body will burn calories to maintain body temperature, breathe, circulate blood, digest food, eliminate wastes, build and repair cells and tissues, and maintain brain and nervous system activity.
Physical activity burns calories beyond the basal metabolic rate. Your muscles use both readily available and stored energy sources in your body. The exercise calories burned during cardiovascular activities such as walking, running, swimming, and cycling depend on the intensity of the exercise, your body weight, and the amount of time you spend exercising.
Moderate-intensity exercises such as brisk walking burn fewer calories per minute than more vigorous-intensity exercises such as running. For example, you can use a walking calorie chart to find out how many calories you can burn per mile based on your weight and speed. Walking burns approximately 90 calories per mile for a 160-pound person. A body that consumes 2500 calories a day, and burns 2500 calories a day will stay at the same weight. A body consuming 2500 calories daily but burning only 2000 will gain weight at the rate of about 1lb a week.
AI Model Details
- Gradient Boosted Regression
- ElasticNet Regression
- Ridge Regression
Distance/Miles
Business Context
“Distance/Mile” let’s you know how far you have walked as an act of daily physical activity. There are several ways to measure your walking distance, with more available than ever before. Mobile Apps, GPS, and computer mapping come to our Recue. The best one to use will depend on whether you are walking outdoors or indoors and how you are using that information.
Walking for 30 minutes covers a distance of 3.8 to 4.6 miles and burns about 125 calories (520 kiloJoules). This amount may not seem like much, but if you walked five days a week within one year you would burn over 32,000 calories which would burn off more than 5 kg of fat. Moreover, the latest scientific evidence shows that you would derive even greater benefits from walking if you burned a minimum of 2000 calories per week by walking around 8 hours a week, spread throughout the week).
Many smart pedometers and fitness bands, such as Fitbit, are linked to apps that have an exercise-tracking function that will use the phone's GPS to map and measure your walk. Besides measuring total distance, you can often review your route on a map Some apps allow you to save and use the same route again. For better distance accuracy, you can walk the same route several times and compare the distance each time. If you are walking in an area with many tall buildings, in a deep valley, or next to a hill, you may see more GPS inaccuracy and loss of signal. Plus, GPS is often lost and doesn't work well indoors. It won't measure your distance on the treadmill because your position isn't changing.
AI Model Details
- Polynomial Regression
- Linear Regression
- Decision Tree Regression
- Artificial Neural Networks
Active Minutes
Business Context
The term “Active Minutes” is defined as “Periods of moderate activity done for 10 minutes or more”. The active minutes measurement tells you when you have spent at least 10 minutes in an activity that burns three times as many calories as you do at rest. When you are at rest, your metabolic equivalents (MET) equal 1. Fitbit uses a level of 3 MET or higher to indicate moderate-intensity exercise. At the 3 MET level, you would be walking briskly or engaging in other exercises that raise your heart rate enough so you are breathing noticeably heavier than usual. Fitbit also uses the 6 MET level to indicate vigorous-intensity exercise.
There are reasons to track your active minutes. Step tracking is a good start. However, there is a difference between “passive steps” and “active steps.” When you’re taking “passive steps,” you are taking a few steps, but only for a minute or two at a time. Walking to another room in your house is an example of “passive steps.” When you’re taking “active steps”, you’re continuously taking steps for more than a few minutes at a time. An example would be when you walk your dog.
Fitbits and other advanced activity monitors and pedometers can sense not only the steps you take but also your cadence to determine whether you are moving faster than an easy walking pace. Simply reaching a goal of 10,000 steps per day doesn't ensure that you have completed 10 continuous minutes of moderate to vigorously intensive exercise. Although you may be moving a lot during, moving at an easy pace will not raise your heart rate sufficiently. Even though you are active, you will not receive the benefits of exercising at an indicated activity level that would reduce your health risks.
AI Model Details
- Linear Regression
- Stepwise Regression
- Lasso Regression
- Gradient Boosted Regression
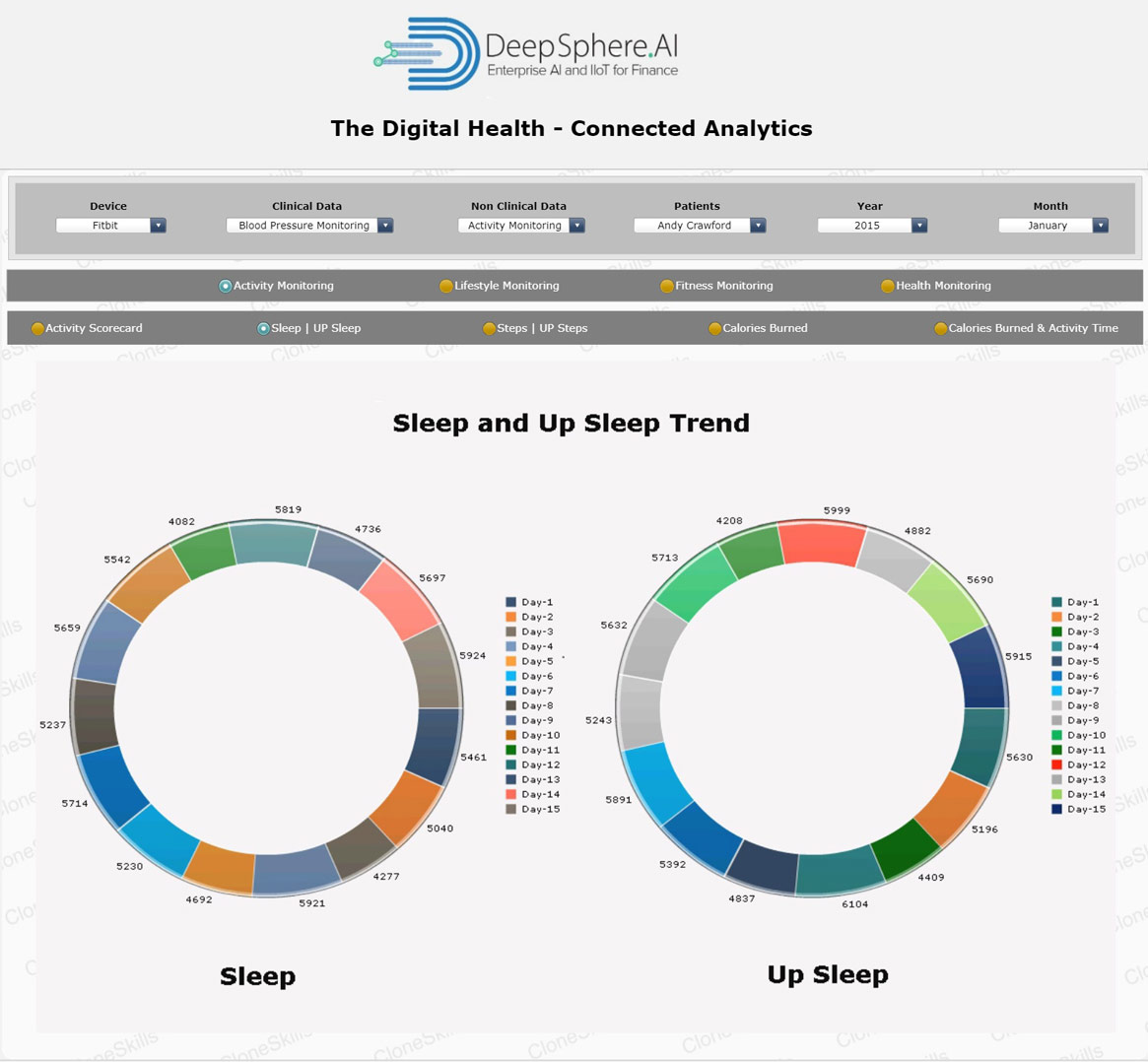
Average Sleep
Business Context
In medical terms “Sleep” is defined as the body's rest cycle. The average amount of sleep for an adult is 7 to 9 Hours. Lack of sleep is stressful to the body. It can cause higher blood pressure, an irregular heart rate and alter metabolism. This in turn leads to spikes in blood sugar that can result in insulin resistance and weight gain. If your sleep is frequently interrupted, you're not getting quality sleep.
The quality of your sleep is just as important as the quantity. The quality of your sleep directly affects your mental and physical health as well as the quality of your waking life. Quality of sleep impacts your productivity, emotional balance, brain and heart health, immune system, creativity, vitality, and even your weight. No other activity delivers so many benefits with so little effort. Scheduling consistent bedtime is important for your overall health and wellbeing because it establishes the foundation to getting the right amount of sleep for you.
Some people claim to feel rested on just a few hours of sleep a night, but their performance may be affected. Research shows that people who do not receive an adequate amount of sleep during many nights do not perform as well on complex mental tasks as those who sleep around seven hours per night. Your body does not just hit each sleep stage once a night, nor does it spend an equal amount of time in each of them. In fact, it cycles through all of these stages multiple times per evening. Each cycle lasts, on average, 90 minutes.
AI Model Details
- Ridge Regression
- Gradient Boosted Regression
- ElasticNet Regression
- Lasso Regression
Weight Loss Factor
Business Context
“Weight - Loss Factor” is a combination of diets that you plan to follow according to how much weight you want to lose and how quickly you want to lose it. In order to continue to eat all your favorite foods without gaining weight, it is important to make sure that your metabolism, liver and colon are working effectively.
For turbo charged weight loss, it is recommend to prepare your body by doing a Master Cleanse. This detox removes toxins which have accumulated in the liver and also clears the colon. During the cleanse you can lose up to 9 pounds and three inches off your waist. However, if detoxing is not for you, then good results can still easily be achieved by following the Quick plan. There is a complete and very detailed list of fat- burning food available. There is also a list of foods which you should choose to eat in moderation. Also there is a list of foods which guarantee weight gain.
Some will be surprised to learn that the top weight-gaining items on this list are doughnuts and pastries. However, some of the other 14-pound packing products are not so obvious. Most of the recipes in the meal plans are comprised of every-day ingredients and are actually very tasty. The nutritional breakdown of most of the recipes is specified and the diet is a low-calorie, low GI type diet.
AI Model Details
- Lasso Regression
- Decision Tree Regression
- Gradient Boosted Regression
Travel Activity
Business Context
“Travelling” is packing up and leaving your comfort zone. In other words, leaving your safety zone and experiencing unknown activities and events, such as a new place, new people who may not understand you, unfamiliar customs are examples of traveling. Traveling is being in the real world. There are 10 vital lessons that traveling will teach you. Travel can be exciting, terrifying, stressful, and more. Additionally, the act of travel can be truly life-changing. There’s no better education than trotting the globe. Certain experiences will surely transform you forever.
Traveling is great in many ways. It captures us with a sense of wanderlust and has us longing for more destinations to visit, cultures to experience, food to eat, and people to meet. As amazing as traveling is, most of us think we need to wait until our later years to really explore a lot of the world. The greatest benefit of traveling is the amount of movement that you will do. You will constantly be on the go, even if you are taking a trip on a cruise. There are sights to see and things to do.
If you have ever wanted to lose weight, explore traveling. Sure, you must eat out more, and you do not always get to control the amount of calories you eat, but you will find it much easier to create a calorie deficit.
AI Model Details
- Stepwise Regression
- Lasso Regression
- Polynomial Regression
- ElasticNet Regression
Entertainment Activity
Business Context
“Entertainment” is a form of activity that holds the attention and interest of an audience or gives pleasure and delight. It can be an idea or a task, but is more likely to be one of the activities or events that have developed over thousands of years specifically for the purpose of keeping an audience's attention. Although the attention of people can be captured by different things, many have different preferences in entertainment. Most of them are recognizable and familiar.
Entertainment Activity has tremendous health Benefits. Being active is great for the body in helping to enhance one’s immune system. Entertainment activities can help prevent or maintain control in some chronic illnesses such as: heart disease, diabetes arthritis, and even some types of cancer. Entertainment activities done over a consistent period can also help in improve overall quality of life and assist in longevity.
Most people pursue entertainment activities because they enjoy them, and many things that we enjoy doing help relieve stress in our lives. Some of these ideas may also help create a calm atmosphere to reduce stress. Examples: Cooking or baking, gardening, taking a walk, singing, reading, or playing a musical instrument.
AI Model Details
- Linear Regression
- Polynomial Regression
- Ridge Regression
- Artificial Neural Networks
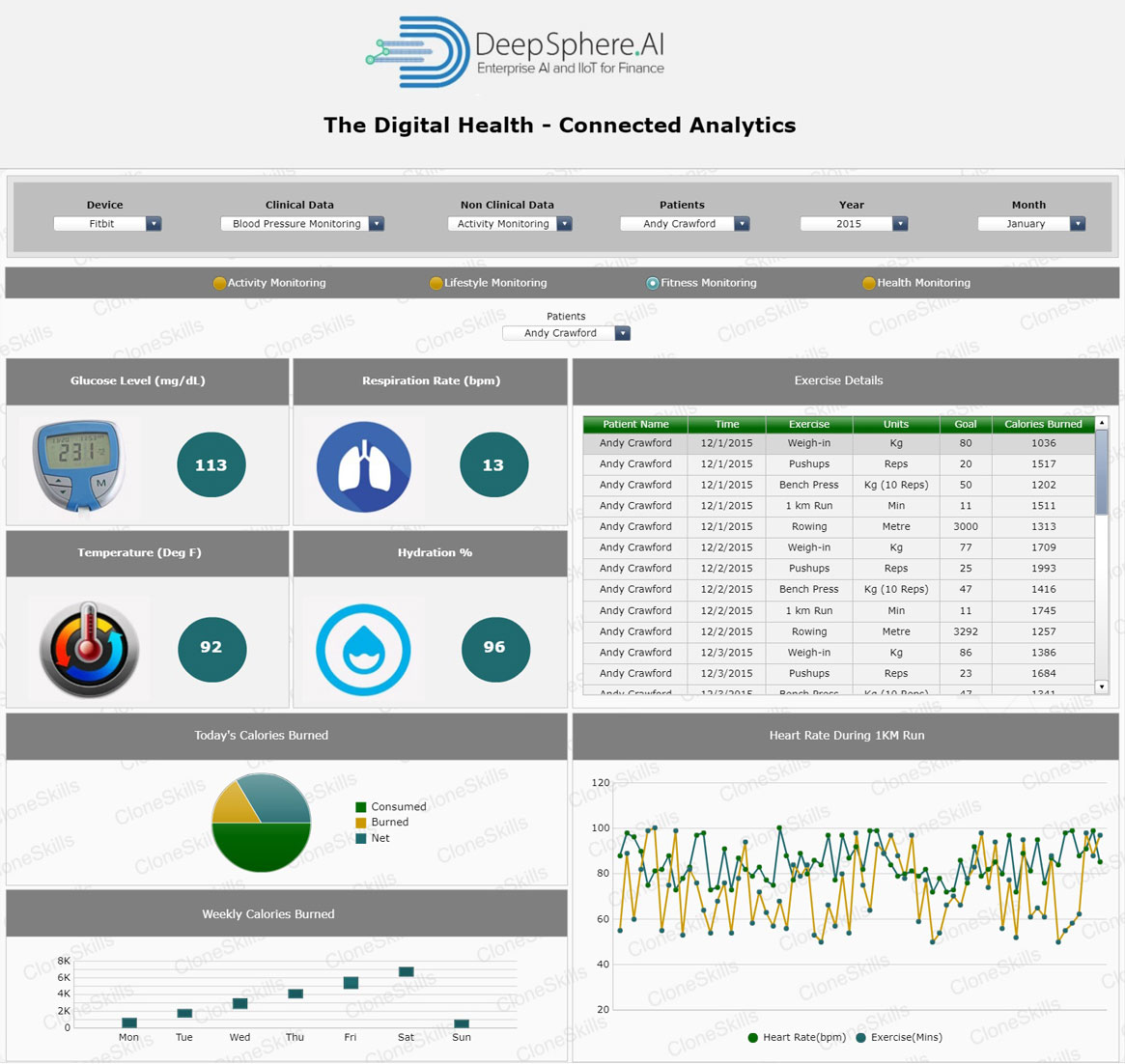
Glucose Level
Business Context
The blood “Glucose Level” is the amount of glucose in the blood. Glucose is a sugar that comes from the foods we eat, and it's also formed and stored inside the body. It is the main source of energy for the cells of our body, and it is carried to each cell through the bloodstream. One needs to keep blood sugar levels within a safe range to reduce the risk of diabetes and heart disease.
Blood glucose monitoring measures the amount of sugar that the blood is transporting during a single instant. People obtain this sugar from the diet. The human body regulates blood glucose levels so that they remain moderate enough glucose to fuel the cells, but not enough to overload the bloodstream. The blood's internal environment must remain stable to support vital bodily functions. Blood glucose levels change throughout the day. After eating, levels rise and then settle after about one hour. They are at their lowest point before the first meal of the day.
It is important to control blood-glucose levels. Many people who live with diabetes do not feel any particular symptoms, unless they are experiencing hyperglycemia (glucose level is too high) or hypoglycemia (glucose level is too low). Hyperglycemia can cause significant damage to some organs, which then leads to complications of diabetes. To avoid the complications of diabetes, one must control blood glucose very well to minimize the risk of hyperglycemia. This will allow one to prevent the complications of diabetes. Monitoring daily glucose levels, also known as self-testing, is an essential part of managing diabetes, just like changing lifestyle habits and taking medication.
AI Model Details
- Gradient Boosted Regression
- Polynomial Regression
- Decision Tree Regression
Respiratory Rate
Business Context
The term “Respiratory Rate (RR) is defined as the number of breaths you take per minute. The normal respiration rate for an adult at rest is 12 to 20 breaths per minute. An RRunder 12 or over 25 breaths per minute while resting is considered abnormal. Among the conditions that can change a normal respiratory rate are asthma, anxiety, pneumonia, congestive heart failure, lung disease, use of narcotics or drug overdose. Respiratory rates change based on many health and activity factors.
Respiratory rate is a vital sign but it is frequently omitted, inaccurately measured and not recorded. A change in RRis often the first sign of deterioration as the body attempts to maintain oxygen delivery to the tissues. Failing to recognize the early signs of deterioration can result in poor outcomes for patients. In a review of abnormal vital signs, it is found that more than half of patients who had a serious adverse event could have been identified as high-risk up to 24 hours previously. It is suggested that early detection and documentation of changes in vital signs, particularly RR could help to detect respiratory failure, which is the most common primary cause of admission to intensive care.
Poor monitoring of RR is a big concern. Hospitals should adopt physiological track-and-trigger systems or early warning scores (EWS) for all adult patients. It can be difficult to measure RR accurately as patients may alter their breathing if they know they are being watched; this can be addressed by techniques such as discreetly counting respirations while appearing to check the radial pulse.
AI Model Details
- ElasticNet Regression
- Polynomial Regression
- Linear Regression
- Artificial Neural Networks
Heart Rate
Business Context
The term “Heart Rate”is defined as number of contractions (beats) of the heart per minute (bpm). The heart rate can vary according to the body's physical needs, including the need to absorb oxygen and excrete carbon dioxide. It is usually equal or close to the pulse measured at any peripheral point. Activities that can provoke change include physical exercise, sleep, anxiety, stress, illness, and ingestion of drugs.
Normal heart rate varies from person to person, but a normal range for adults is 60 to 100 beats per minute. However, a normal heart rate depends on the individual, age, body size, heart conditions, activity level, medication use and even air temperature. Emotions can affect heart rate. For example, getting excited or scared can increase one's heart rate. Most importantly, getting more fit lowers the heart rate by making heart muscles work more efficiently. A well-trained athlete may have a resting heart rate of 40 to 60 beats per minute. Resting heart rate is pulse when you are calmly sitting or lying. It’s best to measure your resting heart rate it in the morning before you get out of bed.
For adults 18 and older, a normal resting heart rate is between 60 and 100 beats per minute (bpm), depending on the person’s physical condition and age. For children ages 6 to 15, the normal resting heart rate is between 70 and 100 bpm. Your resting heart rate is your pulse when you are calmly sitting or lying. It’s best to measure your resting heart rate it in the morning before you get out of bed, according to the AHA. For adults 18 and older, a normal resting heart rate is between 60 and 100 beats per minute (bpm), depending on the person’s physical condition and age.
AI Model Details
Content Goes here
Hydration Rate
Business Context
Hydration is defined as the introduction of additional fluid into the body. Hydration sometimes helps to reduce the concentration of toxic substances in the tissues. “Hydration Rate” is the Rate at which additional fluid is introduced into human body.
Sometimes dehydration requires medical care, administered through different means. The most common method used in the medical facility for hydrating people is administering fluids through an IV or intravenous line, supplying water directly into the bloodstream through a vein. An IV hydrates the body even faster than drinking the water. Injecting fluids directly into tissues to absorb the body is another method used in medical facilities.
There is not a set amount of water that everybody should drink in a given period of time. The amount that it takes to hydrate one person is different from the amount that it would take to hydrate another person. Factors that determine how much water we should drink include body composition, activity level, and the amount of water lost through sweating and breathing.
AI Model Details
- Decision Tree Regression
- Linear Regression
- Artificial Neural Networks
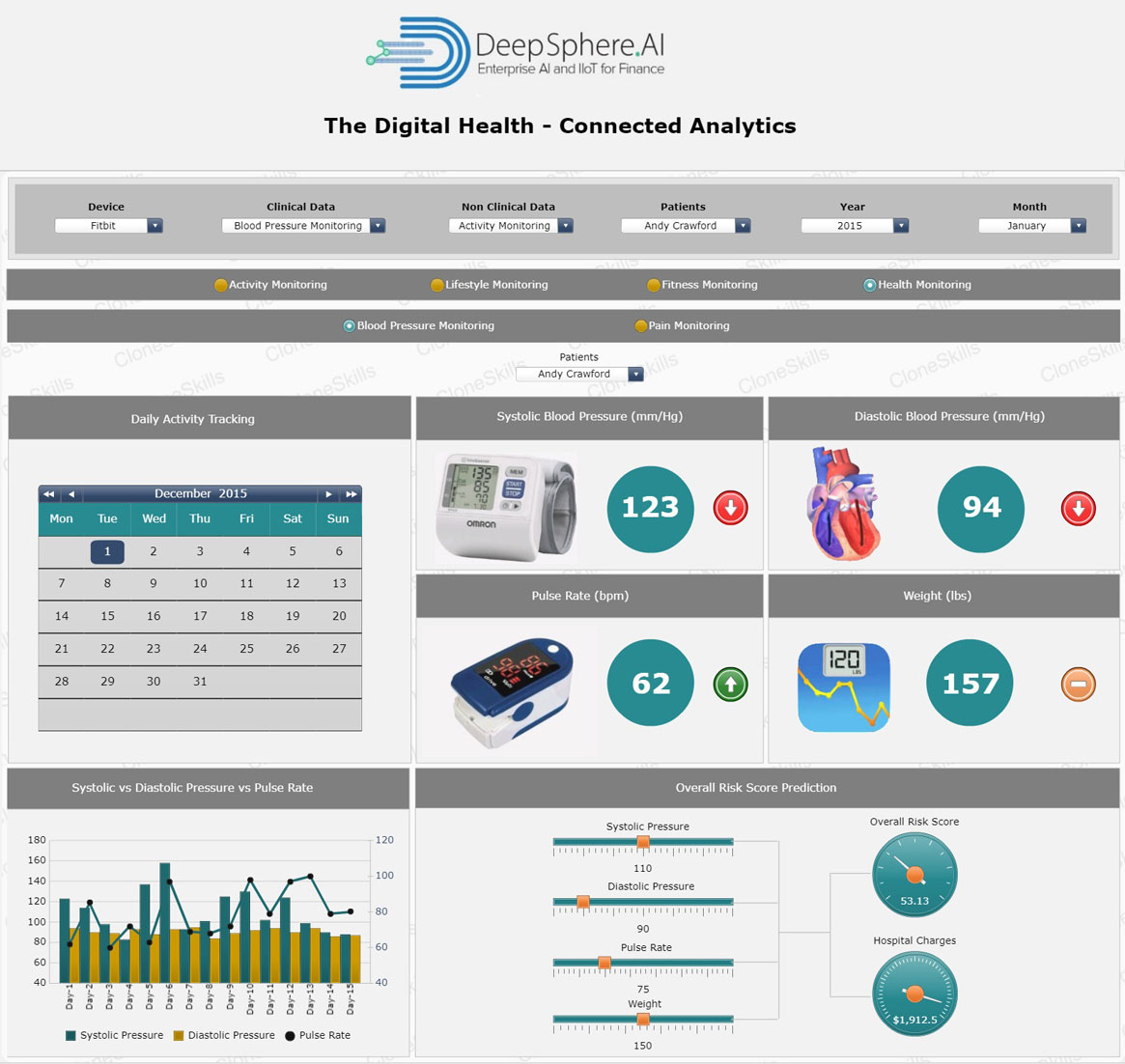
Systolic Blood Pressure
Business Context
When the heart beats, it squeezes and pushes blood through your arteries to the rest of your body. This force creates pressure on those blood vessels, this pressure is called “Systolic Blood Pressure (SBP)”. A normal systolic pressure is below 120. A reading of 140 or more means you have high blood pressure (also called hypertension).
Systolic Blood Pressure can be caused by underlying conditions such as artery stiffness, an overactive thyroid (hyperthyroidism) or diabetes. Occasionally, it can be caused by heart valve problems. It is the most common form of high blood pressure in people older than age 65, but it is possible for younger people to be affected by this type of high blood pressure as well. High systolic pressure is as important as high diastolic pressure and even more important in people older than age 50. Having a high systolic pressure for a long period of time can increase your risk of having significant cardiovascular problems, such as a heart attack or stroke.
The recommended goal for systolic pressure for adults younger than age 65 with a 10 percent or higher risk of developing cardiovascular disease is less than 130 mm Hg. For healthy adults who are age 65 or older, the recommended treatment goal for systolic pressure is also less than 130 mm Hg. high blood pressure will need to be controlled with medications in order to prevent health problems. However, if your treatment lowers your diastolic pressure too much, you could be more likely to have a heart attack or stroke
AI Model Details
- Ridge Regression
- Linear Regression
- Polynomial Regression
- Lasso Regression
Diastolic Blood Pressure
Business Context
“Diastolic Pressure” is defined as the pressure the blood exerts within the arteries in between heartbeats, that is, when the heart is not actively ejecting blood into the arteries. After the heart is finished contracting, the cardiac ventricles relax momentarily so that they can be refilled with blood, in preparation for the next contraction. This period of ventricular relaxation is called “Diastole.”A normal Diastolic Blood Pressure during quiet rest is 80 mmHg or below.
Diastolic Blood Pressure may be seen with dehydration or with bleeding episodes, or if the arteries become abnormally dilated. Diastolic Blood Pressure around 90 and 60 is good in olderer people. Once it dips below 60, people feel uncomfortable. A lot of elderly people with low diastolic pressures get tired or dizzy and have frequent falls. Obviously, none of that is good news for people who are older, who potentially have brittle bones and other issues.
Coronary arteries are fed during the diastolic phase. If you have a low diastolic pressure, it means you have a low coronary artery pressure, and that means your heart is going to lack blood and oxygen. That is what is called ischemia, and that kind of chronic, low-level ischemia may weaken the heart over time and potentially lead to heart failure.
AI Model Details
- Stepwise Regression
- Decision Tree Regression
- Lasso Regression
Pulse Rate
Business Context
“Pulse Rate” is defined as the number of times your heart beats per minute. Pulse rates vary from person to person. Your pulse is lower when you are at rest and increases when you exercise (because more oxygen-rich blood is needed by the body when you exercise). A normal pulse rate for a healthy adult at rest ranges from 60 to 80 beats per minute.
Women tend to have faster pulse rates than men. Your pulse can be measured by firmly but gently pressing the first and second fingertips against certain points on the body most commonly at the wrist or neck (but can also be measured at the bend of the arms, in the groin, behind the knees, inside the ankles, on the top of the feet or at the temple area of the face) then counting the number of heart beats over a period of 60 seconds.
A faster-than-average pulse can indicate health problems as infection, dehydration, stress, anxiety, a thyroid disorder, shock, anemia or certain heart conditions. Some medications, especially beta blockers and digoxin, can slow your pulse. A lower heart rate is also common for people who get a lot of exercise or are athletic. If checking your pulse, your pulse rate should not be routinely less than 60 beats per minute. The beats also should be equally spaced out, not excessively strong (would indicate a heart that is working hard), and no beats should be missed.
AI Model Details
Content Goes here
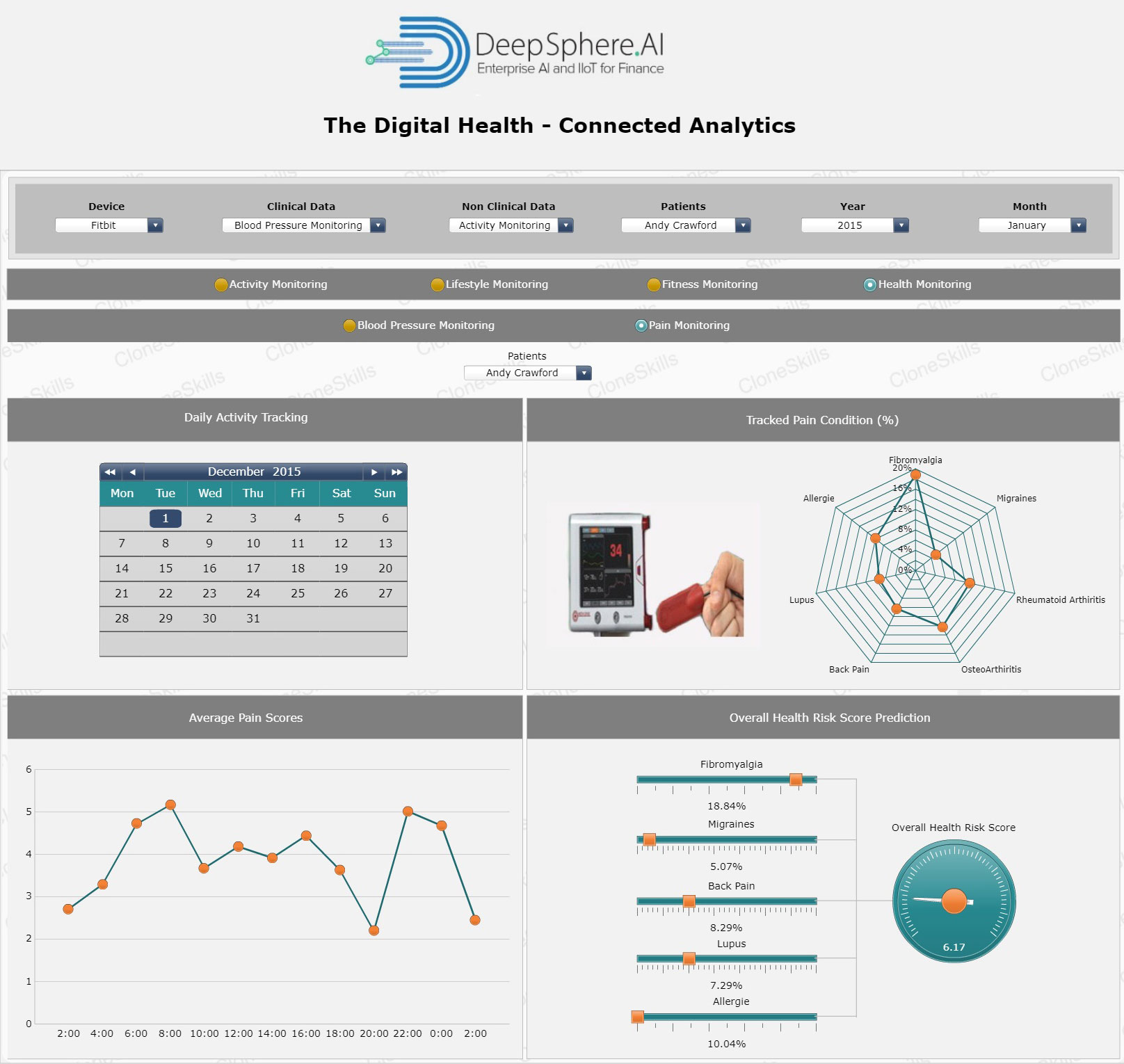
Pain Condition
Business Context
Pain is a distressing feeling often caused by intense or damaging stimuli or an unpleasant sensory and emotional experience associated with actual or potential tissue damage or terms of such damage. Pain motivates an individual to withdraw from damaging situations, to protect a damaged body part while it heals, and to avoid similar experiences in the future.
Pain Conditions are of two types: Chronic and Acute. Chronic pain is any pain lasting more than 12 weeks. Whereas acute pain is a normal sensation that alerts us to possible injury, chronic pain is very different. Chronic pain persists often for months or even longer. Chronic pain may arise from an initial injury, such as a back sprain, or an ongoing cause, such as illness. However, there may also be no clear cause. Other health problems, such as fatigue, sleep disturbance, decreased appetite, and mood changes often accompany chronic pain. Chronic pain may limit a person’s movements, which can reduce flexibility, strength, and stamina. This difficulty in carrying out important and enjoyable activities may lead to disability and despair.
Chronic pain affects 1 in 5 people. It can affect all ages and all parts of the body. It isn't possible to tell in advance whose pain will become chronic. But we know that people are more likely to develop chronic pain during or after times of stress or unhappiness. People can also experience chronic pain even after usual medical tests don’t provide an answer.
AI Model Details
- Lasso Regression
- Polynomial Regression
- Gradient Boosted Regression
- Decision Tree Regression
Patient Health Risk
Business Context
Patient Health Risk is any attribute, characteristic, or exposure of an individual that increases the likelihood of developing a disease or injury. Some examples of the more important risk factors are underweight, unsafe sex, high blood pressure, tobacco, alcohol consumption, and unsafe water, sanitation, and hygiene. Patient health risks are all around us. Obesity boosts the odds you will get diabetes. Smoking increases your risk for many cancers. When forecasting revenue for the consumer industry, you predict the market size and use current market share and competitor analysis. When forecasting revenue for any service industries, you estimate the headcount and use the income for employee trends.
Patient health risks can be confusing. However, knowing the risks you and your family may face can help you find ways to avoid health problems. It can also keep you from fretting over unlikely threats. By knowing the risks and benefits of medical treatment, you and your doctor can make more informed decisions. A health risk is a chance or likelihood that something will harm or otherwise affect your health. A risk is not necessarily bad. It is just a possibility. Several characteristics, called risk factors determine whether your health risks are high or low.
Your health risk factors include age, sex, family health history, lifestyle, and more. You cannot change some risk factors such as genes or ethnicity. However, there are risk factors that you can change. You can choose to exercise, eat a balanced diet, and wear a seatbelt.
Model Details
- Logistic Regression
- Naïve Bayes
- Decision Tree
- Artificial Neural Networks
Patient Financial Risk
Business Context
Patient Financial Risk describes the health or potential financial loss of a patient. There are many dimensions to financial risks, such as the amount of your savings, plan for retirement, and the amount of income you are spending on fixed or non-discretionary expenses. There are several ways to measure an individual’s financial health. A person’s savings and overall net worth represent the monetary resources at their disposal for current or future use. Credit card debt, mortgages, and student loans can impact financial health. The financial health risk is not a static figure. It changes based on an individual’s liquidity and assets, as well as the fluctuation of the price of goods and services.
To get a better grasp of financial health, it might help to ask yourself a few key questions consider this a self-assessment of your financial health:
- How prepared are you for unexpected events? Do you have an emergency fund?
- What is your net worth? Is it positive or negative?
- Do you have the things you need in life? How about the things you want?
- What percent of your debt would you consider high interest, such as credit cards? Is it more than 50%?
- Are you actively saving for retirement? Do you feel you’re on track to meet your long-term goal?
- Do you have enough insurance coverage—whether it be health or life?
Model Details
- Naïve Bayes.
- Random Forests.
- Decision Tree Classifier.
- Logistic Regression.
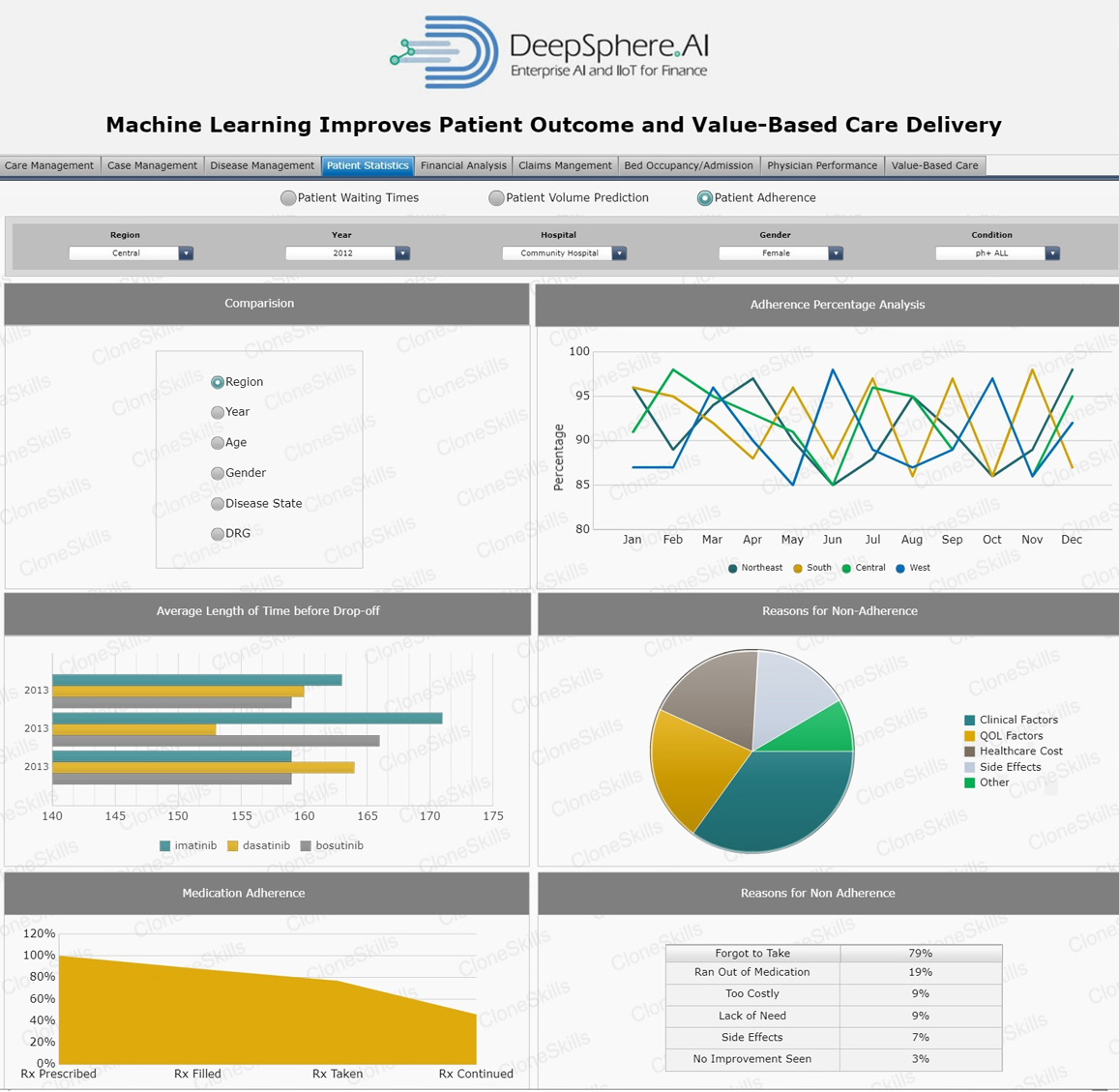
Patient Adherence
Business Context
Patient Adherence is typically the percentage of patients taking medications correctly and as prescribed, particularly at the right time(s) daily and getting prescriptions refilled in a timely fashion is an example of patient adherence.
Health literacy and costs are barriers to medication adherence and health inequalities. There is strong evidence that education and physical health are correlated. Poor medication adherence can adversely affect the trajectory of the disease, requiring expensive medical services. Unfortunately, poor adherence leads to both suboptimal clinical benefits for patients and the inefficient use of health care resources. Due to many factors and complexities underlying poor drug adherence, interventions to increase patient drug adherence have proven to be a challenge.
Model Details
- Lasso Regression
- ElasticNet Regression
- Ridge Regression
Patient Behavioral Patterns
Business Context
Adapting new behaviors is essential for patients and healthcare providers. Some patients succeed; others struggle. Nevertheless, everyone can change behavior. We are natural learners. As infants, we first learned to crawl. Then we learned to walk. Learning throughout adulthood and changing behavior is essential. Some changes in behavior are simple and happen almost automatically – like adjusting to a new phone or taking a new route on the way to work.
Some situations in life require a drastic change in behavior that can keep people in a constant state of turmoil and struggle. For patients, dealing with a chronic condition may require a greater awareness of nutrition, medications, and activity level. Healthcare professions must adapt to new medical practices and abandon familiar and trusted habits. Otherwise, frustration is the likely outcome. Making new changes in behavior is possible when one understands all of the steps to make a positive change. When one considers one level of change, behavior modification fails. For instance, some patients might know “why” they should take care of themselves in a certain way but not understand “what” they should do or how to do it. A patient may fail to grasp the meaning of good hygiene, even though a health professional explained the importance of good hygiene.
Model Details
- Stepwise Regression
- Gradient Boosted Regression
- Decision Tree Regression
- Artificial Neural Networks
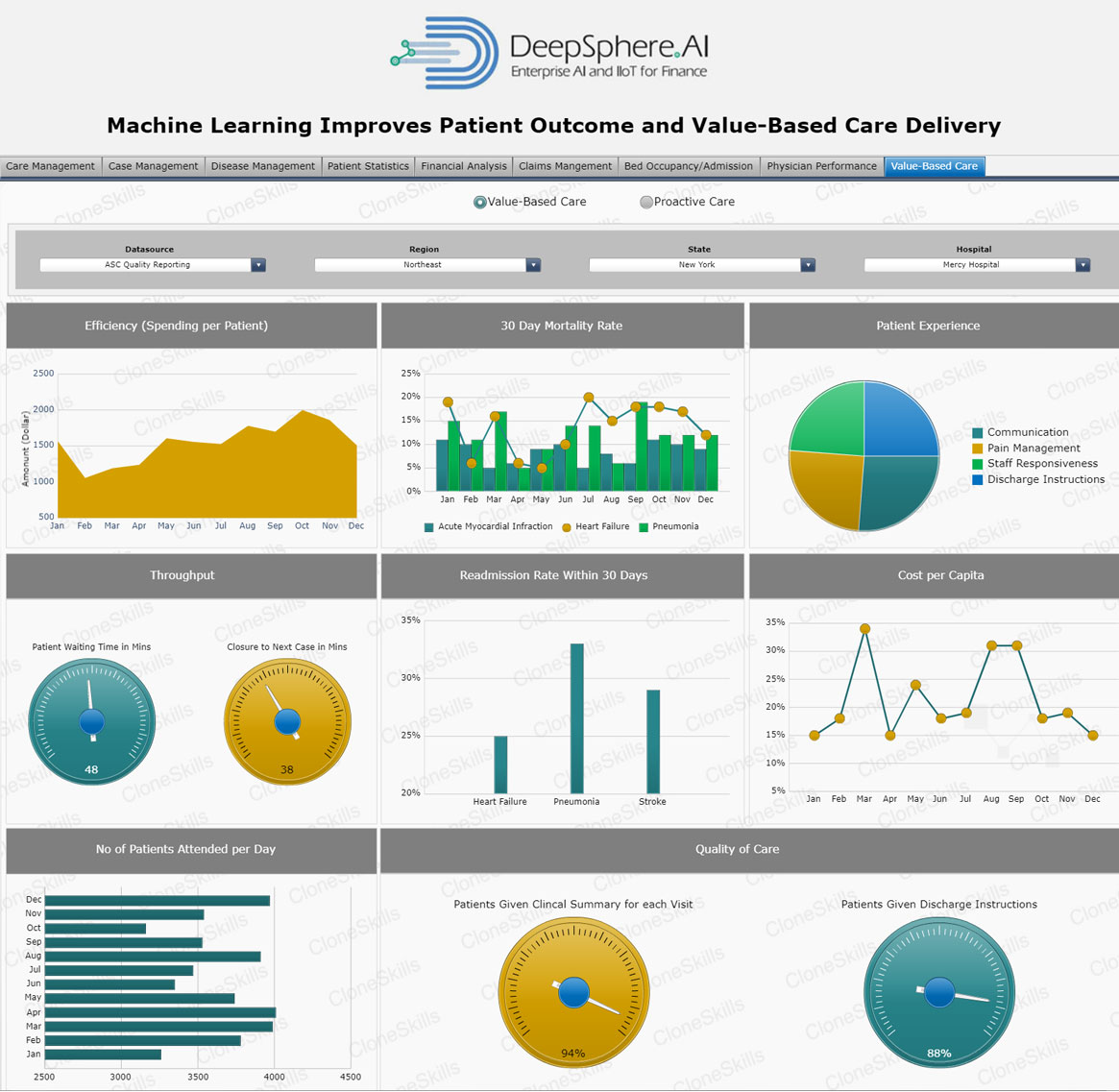
Value Based Care Delivery
Business Context
Value-Based Care is the extent to which health care professionals provide quality care for patients, and better health at a lower cost To achieve this, health care must be safe, effective, timely, efficient, equitable, and people-centered.
Health facilities often struggle to provide the rapid emergency care needed to manage maternal complications and care for small and sick newborns. Common causes include inadequate or unhygienic infrastructure; lack of competent, motivated staff; lack of availability or poor quality of medicines; poor compliance to evidence-based clinical interventions and practices; poor documentation and use of information. Improving the quality of care and patient safety are, therefore, critical to accelerating reductions in maternal and newborn mortality.
Value-Based Care is also a key component of health rights and the route to equity and dignity for women and children. To achieve universal health coverage, delivering health services that meet quality criteria is essential.
Model Details
- Linear Regression
- Polynomial Regression
- Ridge Regression
Pay for Performance
Business Context
Pay for Performance (P4P), also known as value-based payment, comprises payment models that attach financial incentives/disincentives to provider performance. Pay for Pay is part of the overall national strategy to transition healthcare to value-based medicine. While it still utilizes the fee-for-service system, it nudges providers toward value-based care because it ties reimbursement to metric-driven outcomes, proven best practices, and patient satisfaction, thus aligning payment with value and quality.
Pay for performance systems link compensation to measures of work quality or goals. Current methods of healthcare payment may actually reward less-safe care, since some insurance companies will not pay for new practices to reduce errors, while physicians and hospitals can bill for additional services that are needed when patients are injured by mistakes. However, early studies showed little gain in quality for the money spent, as well as evidence suggesting unintended consequences, like the avoidance of high-risk patients, when payment was linked to outcome improvements.
The objective of the Hospital Value-Based Purchasing Program is to improve healthcare quality and patient experience by leveraging financial carrots and sticks to encourage hospitals to follow established best clinical practices and improve patient satisfaction scores via Hospital Consumer Assessment of Healthcare Providers and Systems Survey.
Model Details
- Ridge Regression
- Polynomial Regression
- Stepwise Regression
- ElasticNet Regression
Readmission Rate
Business Context
Readmission Rate is the percentage of patient admission to a hospital within 30 days when discharged from an earlier hospital stay. Patients transferred to another hospital for long term care will not count as readmission. The percentage of admitted patients who return to the hospital within seven days of discharge will stay the same or decrease with changes to improve patient flow through the system.
Percentage of readmitted patients is an important balancing measure to indicate if changes to patient flow through the system are negatively affecting care. While some readmissions are part of the planned care and are desirable, others may be indications of a quality issue related to shortened length of stay and premature discharge.
Tracking the number of patients who experience unplanned readmissions to a hospital after a previous hospital stay is one category of data used to evaluate the quality of hospital care. It’s important to note that unplanned hospital readmissions may or may not be related to the previous visit, and some unplanned readmissions aren’t preventable. Whatever the reason, insurance companies and other payers sometimes view unplanned hospital readmissions as wasteful spending.
Model Details
- ElasticNet Regression
- Decision Tree Regression
- Artificial Neural Networks
- Recurrent Neural Networks
Discharge Rate and LOS
Business Context
Length of Stay (LOS) is the length of an inpatient episode of care, calculated from the day of admission to the day of discharge, based on the number of nights spent in the hospital. Patients admitted for one day are discharged on that same day.
LOS is the amount of time of a new patient to a nursing center from a hospital. New admissions refer to anyone admitted from a hospital with no assessments within the 100 days before the admission assessment. The days between admission and discharge from a hospital determines each person’s LOS. A patient not discharged within 120 days receives a designation of 120 days, even if he or she stays after 120 days. The calculation of LOS is within 12 months. It is rolling and updated quarterly.
Hospital Discharge Rate is the number of patients leaving a hospital after receiving care, particularly for those who stay at least one night. This figure includes deaths in the hospital following inpatient care, excluding same-day discharges, measured per 100,000 inhabitants..
Hospital care is for people who need a high level of medical attention. It is also expensive and often uncomfortable. Being in the hospital also exposes one to the possibility of infection, particularly those with a weak immune system.
Model Details
- Polynomial Regression
- Lasso Regression
- Ridge Regression
- Gradient Boosted Regression
- Lasso Regression
- ElasticNet Regression
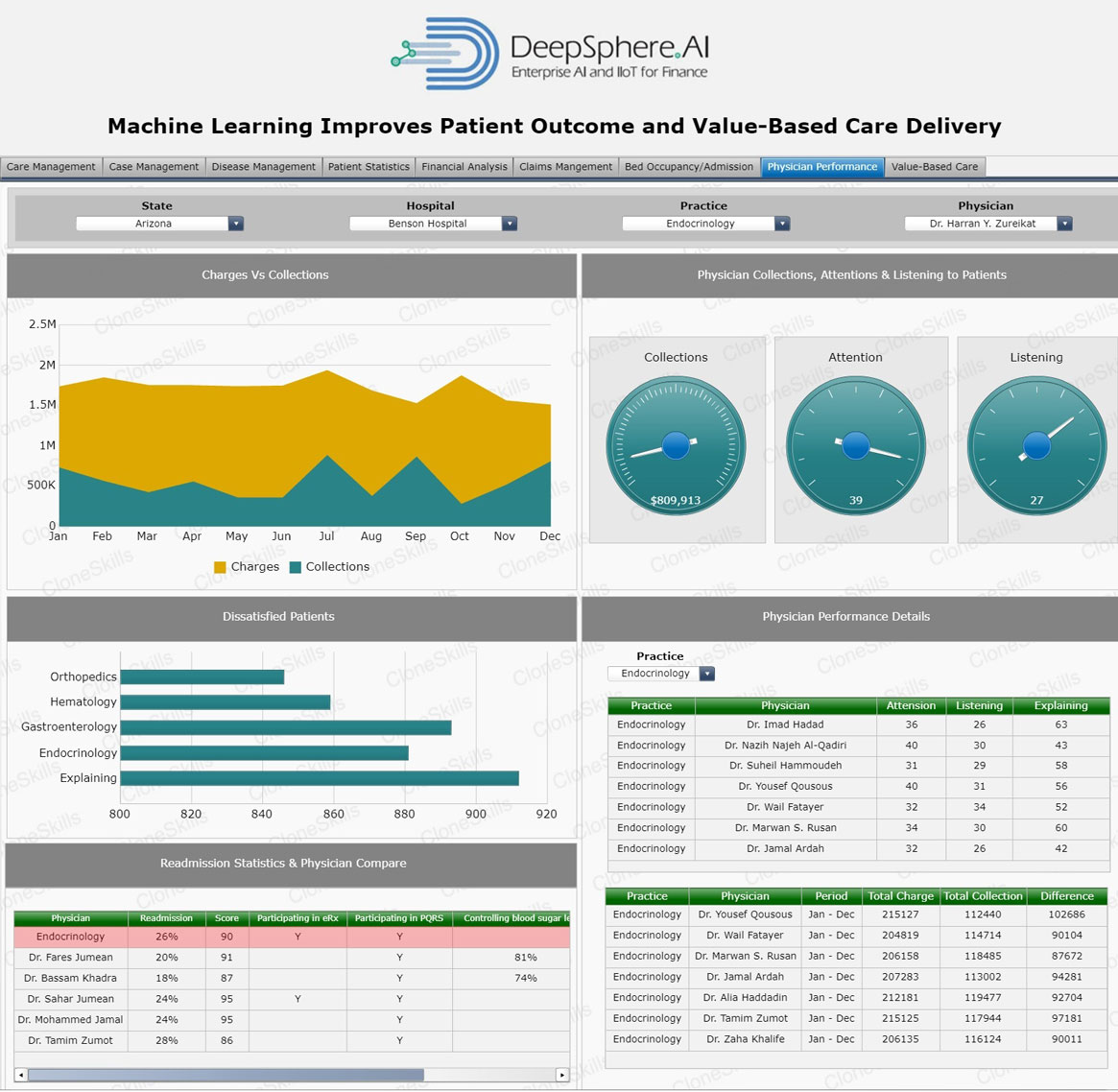
Physician Performance
Business Context
Physician Performance is the measurement of a physician’s charges and collections. Physician Charges refer to the full, non-discounted fees charged for all services provided before the application of any contractual, charitable, courtesy, bad debt, or other adjustments. The collection of full charges for physicians performing similar work is rare on an even playing field.
Physician Collections is the actual cash received for services. In many practices, the recording of received cash is the actual revenue. It is also relatively simple to capture this information by the physician. However, this method may not accurately reflect the work performed.
Model Details
- Linear Regression
- Decision Tree Regression
- Gradient Boosted Regression
- Artificial Neural Networks
Financial Forecasting on Claims
Business Context
Financial Forecasting on Claims measures inpatient, outpatient claims, and account receivable days. Inpatient is a person admitted to an approved hospital or day surgery facility and discharged following treatment. A person admitted as a private patient is eligible to receive benefits for services listed in a chosen level of hospital cover. This procedure is called “Inpatient Claims.”
An outpatient is one who has received medical treatment at a doctor’s surgery or emergency department without admission to a hospital. Private health insurance does not cover this type of treatment. These services may be eligible for claims through Medicare. Services include X-rays, blood tests, and MRIs. This procedure is “Outpatient Claims.”
In health economics, Outstanding Accounts Receivables (AR) Days is the average number of days to collect payments due to the practice. For example, if a patient is charged $280,000 within the past six months, and if there were 182 days in those months, the average daily revenue is $1,538. Then the total accounts receivable is $70,000. The days in Accounts Receivable are 45.5 because it takes an average of 45.5 days to collect patients’ payments.
Days in accounts receivable measure the amount of time between patient discharge and when payment is made. This directly impacts cash flows for the facility. The quicker the turnover in accounts receivable, the less cash is available somewhere else.
Model Details
- Stepwise Regression
- Linear Regression
- Polynomial Regression
- ElasticNet Regression
- Lasso Regression
- Artificial Neural Networks
Fraud Detection
Business Context
Fraud Detection is a set of activities to prevent the taking of money or property through pretenses. Fraud is typically an act which involves many repeated methods. Searching for patterns is the general focus of fraud detection. Fraudulent healthcare claims increase the burden on society. Therefore, healthcare fraud detection is paramount. Generally, healthcare fraud is difficult to detect. The following are typical examples of healthcare fraud techniques used by health care providers and patients:
- Billing for services not provided
- Administering additional tests, treatments, or equipment not medically necessary
- Providing unnecessary and expensive equipment (up-coding)
- Using multiple billing for services
- Unbundling or billing separately for laboratory tests performed together to receive higher reimbursements
- Charging more than peers for the same services
Healthcare fraud detection involves account auditing and detective investigation. Careful account auditing can reveal suspicious providers and policyholders. While auditing every individual claim is the best procedure, this not practical nor feasible. Furthermore, auditing providers without concrete evidence is challenging. A practical approach is to develop shortlists for scrutiny and perform auditing on providers and patients in the shortlists.
Model Details
- Ridge Regression
- Decision Tree Regression
- Lasso Regression
- Stepwise Regression
Case & Disease Management
Business Context
Case management is a collaborative process that assesses, monitors, plans, and evaluates the necessary services to maintain client health and human services concerns through advocacy, communication, and resource management with cost-effective interventions and outcomes. Case management services thrive in a climate that allows direct communication between the case manager, the client, and appropriate service personnel, to optimize the outcome for everyone.
Disease management is an approach to healthcare that teaches patients how to manage a chronic disease. Patients learn to take responsibility for understanding how to take care of themselves. They learn to avoid potential problems and exacerbation, or worsening, of their health problem. Example: One step in teaching disease management to a diabetes patient is to show him or her how to keep blood sugar levels within a healthy range.
Model Details
- Polynomial Regression
- Lasso Regression
- ElasticNet Regression
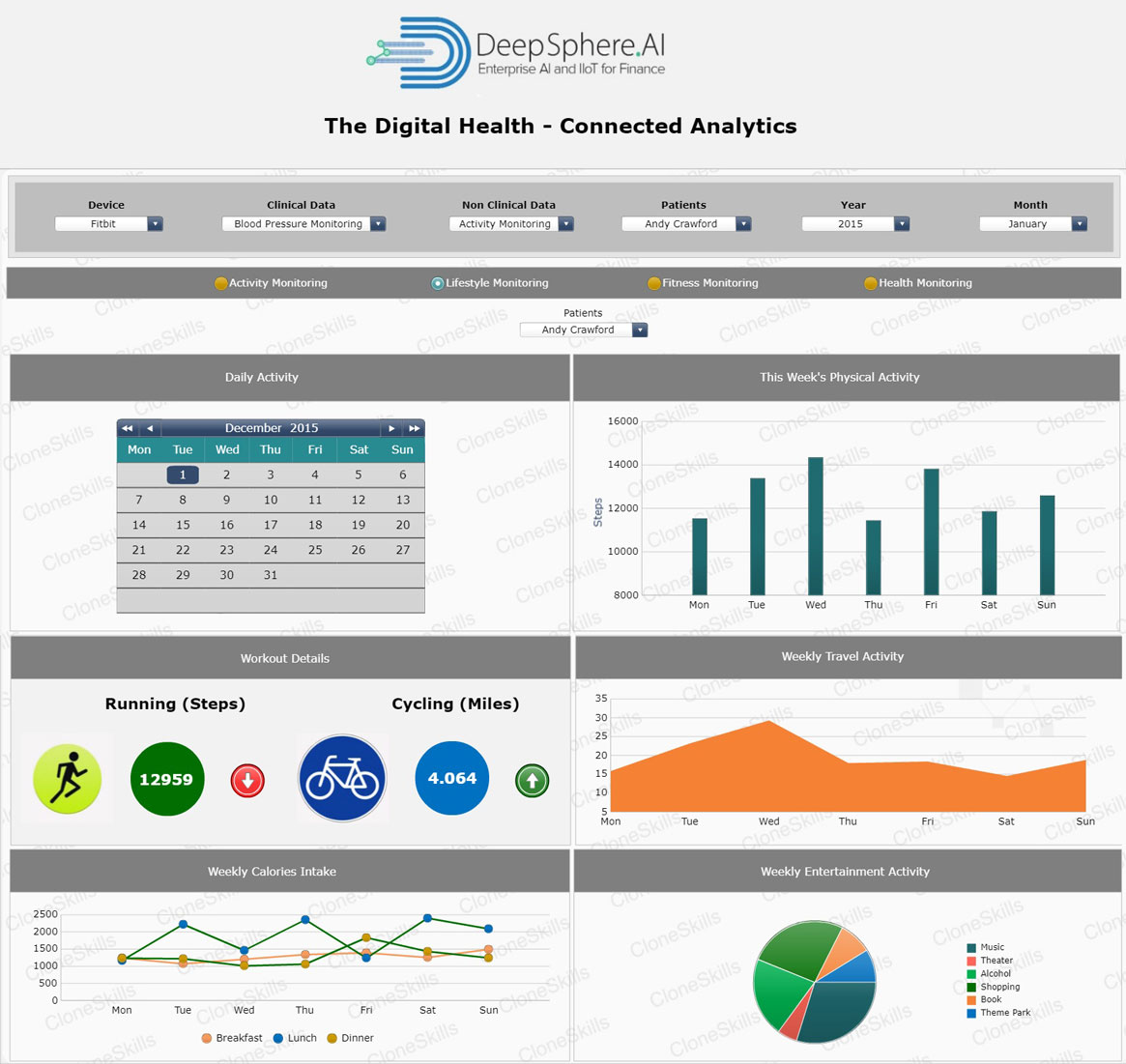
Lifestyle Monitoring
Business Context
Lifestyle Monitoring is the measure of a weight determined by weight loss patterns, travel patterns, and entertainment activities. Weight-Loss Factor is a combination of diets that one plans to follow to lose weight quickly. Eating all of one's favorite foods requires that one's metabolism, liver, and colon work effectively.
Travelling is packing up and leaving a comfort zone. Examples of traveling include leaving a safety zone and experiencing unknown activities and events, such as a new place, new people with unfamiliar customs. Traveling is being in the real world. It can be exciting, terrifying, stressful, and more. Additionally, the act of travel can be truly life-changing.
Entertainment is a form of activity that holds the attention and interest of an audience or gives pleasure and delight. Although it can be an idea or a task, it is more likely to be one of the activities or events that have developed over thousands of years to keep an audience's attention. Although preferences in entertainment vary, most are recognizable.
Model Details
- Linear Regression
- Polynomial Regression
- Ridge Regression
- Artificial Neural Networks
Fitness Monitoring
Business Context
Fitness Monitoring is the measurement of glucose level, respiration, heart, and hydration rate. The blood “Glucose Level” is the amount of glucose in the blood. Glucose is a sugar that comes from the foods one eats. It is formed and stored inside the body. Glucose is the main source of energy for the cells in the body, carried through the cells in the bloodstream. One needs to keep blood sugar levels within a safe range to reduce the risk of diabetes and heart disease.
Respiratory Rate (RR) is the number of breaths one takes per minute. The normal respiration rate for an adult at rest is 12 to 20 breaths per minute. A respiratory rate that is under 12 breaths per minute or over 25 breaths per minute while resting is abnormal. Asthma, anxiety, pneumonia, congestive heart failure, narcotics, or drug overdose are conditions that can change respiration. Activity levels influence the respiration rate.
Heart Rate is the number of contractions (beats) of the heart per minute (bpm). The heart rate can vary according to the body's physical needs, including the need to absorb oxygen and excrete carbon dioxide. It is usually equal or close to the pulse measured at any peripheral point. Activities that can provoke change include physical exercise, sleep, anxiety, stress, illness, and the ingestion of drugs.
Hydration is the introduction of additional fluid into the body. Hydration sometimes helps to reduce the concentration of toxic substances in the tissues. Hydration Rate is the measure of fluids introduced in the body.
Model Details
- ElasticNet Regression
- Polynomial Regression
- Linear Regression
- Artificial Neural Networks
Health Monitoring
Business Context
Health monitoring or patient monitoring is the process of using technology to observe patients in nonclinical environments such as the home. When incorporating health care in the management of diseases, it can significantly improve the quality of life for patients. Therefore, it is not a surprise that this technology is growing in popularity.
Although health monitoring is a diverse field, the associated technologies can share some similar components. A monitoring device, first of all, requires a sensor that can measure specific physiological data and wirelessly communicate this information to both the patient and healthcare professionals. Health monitoring can aid patients with numerous conditions, such as diabetes or heart conditions. Those at risk of diabetes may need to control their weight, blood pressure, and blood glucose levels to remain healthy.
Health monitoring provides patients more power to keep an eye on their health. Since technology alerts both patients and healthcare professionals about slight physiological changes, early detection of potentially dangerous conditions is possible. Even though the costs are high, and the technology still needs to be refined, remote monitoring is likely to become a core component of the preventive healthcare of the future.
Model Details
- Lasso Regression
- Polynomial Regression
- Gradient Boosted Regression
- Decision Tree Regression